#76 – Tara Kirk Sell on COVID-19 misinformation, who’s done well and badly, and what we should reopen first
#76 – Tara Kirk Sell on COVID-19 misinformation, who’s done well and badly, and what we should reopen first
By Robert Wiblin and Keiran Harris · Published May 8th, 2020
On this page:
- Introduction
- 1 Highlights
- 2 Articles, books, and other media discussed in the show
- 3 Transcript
- 3.1 The interview begins [00:01:43]
- 3.2 Misinformation [00:05:07]
- 3.3 Who has done well during COVID-19? [00:22:19]
- 3.4 Guidance for governors on reopening [00:34:05]
- 3.5 Collective Intelligence for Disease Prediction project [00:45:35]
- 3.6 What else is CHS trying to do to address the pandemic? [00:59:51]
- 3.7 Deaths are not the only health impact of importance [01:05:33]
- 3.8 Policy change for future pandemics [01:10:57]
- 3.9 Emerging technologies with potential to reduce global catastrophic biological risks [01:22:37]
- 3.10 Careers [01:38:52]
- 3.11 Good news about COVID-19 [01:44:23]
- 3.12 Rob's outro [01:51:02]
- 4 Learn more
- 5 Related episodes
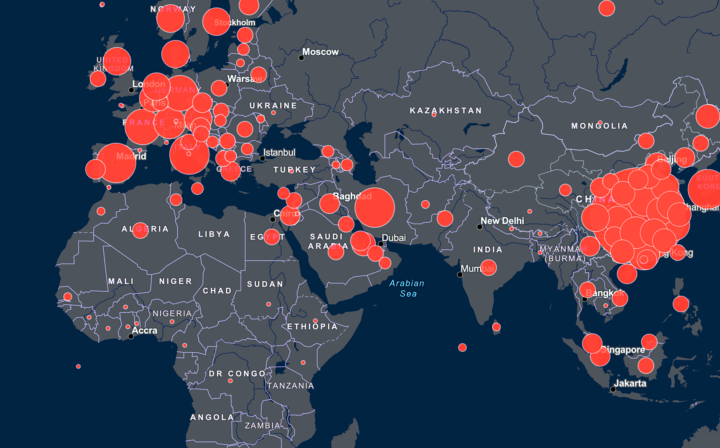
Amid a rising COVID-19 death toll, and looming economic disaster, we’ve been looking for good news — and one thing we’re especially thankful for is the Johns Hopkins Center for Health Security (CHS).
CHS focuses on protecting us from major biological, chemical or nuclear disasters, through research that informs governments around the world. While this pandemic surprised many, just last October the Center ran a simulation of a ‘new coronavirus’ scenario to identify weaknesses in our ability to quickly respond. Their expertise has given them a key role in figuring out how to fight COVID-19.
Today’s guest, Dr Tara Kirk Sell, did her PhD in policy and communication during disease outbreaks, and has worked at CHS for 11 years on a range of important projects.
Last year she was a leader on Collective Intelligence for Disease Prediction, designed to sound the alarm about upcoming pandemics before others are paying attention. Incredibly, the project almost closed in December, with COVID-19 just starting to spread around the world — but received new funding that allowed the project to respond quickly to the emerging disease.
She also contributed to a recent report attempting to explain the risks of specific types of activities resuming when COVID-19 lockdowns end.
It’s not possible to reach zero risk — so differentiating activities on a spectrum is crucial. Choosing wisely can help us lead more normal lives without reviving the pandemic.
Dance clubs will have to stay closed, but hairdressers can adapt to minimise transmission, and Tara (who happens to also be an Olympic silver medalist swimmer) suggests outdoor non-contact sports could resume soon at little risk.
Her latest work deals with the challenge of misinformation during disease outbreaks.
Analysing the Ebola communication crisis of 2014, they found that even trained coders with public health expertise sometimes needed help to distinguish between true and misleading tweets — showing the danger of a continued lack of definitive information surrounding a virus and how it’s transmitted.
The challenge for governments is not simple. If they acknowledge how much they don’t know, people may look elsewhere for guidance. But if they pretend to know things they don’t, or actively mislead the public, the result can be a huge loss of trust.
Despite their intense focus on COVID-19, researchers at the Center for Health Security know that this is not a one-time event. Many aspects of our collective response this time around have been alarmingly poor, and it won’t be long before Tara and her colleagues need to turn their mind to next time.
You can now donate to CHS through Effective Altruism Funds. Donations made through EA Funds are tax-deductible in the US, the UK, and the Netherlands.
Tara and Rob also discuss:
- Who has overperformed and underperformed expectations during COVID-19?
- When are people right to mistrust authorities?
- The media’s responsibility to be right
- What policies should be prioritised for next time
- Should we prepare for future pandemic while the COVID-19 is still going?
- The importance of keeping non-COVID health problems in mind
- The psychological difference between staying home voluntarily and being forced to
- Mistakes that we in the general public might be making
- Emerging technologies with the potential to reduce global catastrophic biological risks
Get this episode by subscribing to our podcast on the world’s most pressing problems and how to solve them: type 80,000 Hours into your podcasting app. Or read the transcript below.
Producer: Keiran Harris.
Audio mastering: Ben Cordell.
Transcriptions: Zakee Ulhaq.
Highlights
Misinformation
Misinformation is something that we see all the time and we’ve also seen these disinformation campaigns that have really started to move into public health. There was a paper in AJPH about Russian trolls and the vaccine debate. So I’m not surprised that we’ve seen this level of misinformation and disinformation in this outbreak. I’m glad that people are paying more attention to it. I think it is a huge opportunity to sow division in the American public and lead to a lot of lack of trust which to me is really concerning. So I think the themes we saw for the Ebola outbreak, we see those exact same things now. You could almost just take the disease name out and replace it and you see many of those same themes. So that wasn’t surprising. But the extent to which we’re seeing it, I guess, is something that’s new and interesting.
The difficulty of writing good forecasting questions
It’s hard to write these questions because you have to sort of think, “Okay, what could the range of outcomes be?” And the outbreak was moving so quickly and we were finding more bad things happening. And so I think that it comes down to the fact that one limitation of these platforms is being able to write a good question. And it’s very, very difficult to do that. And also, the other thing is that when you actually score it at the end, you need to have a clear outcome, right?
Because otherwise your forecasters are really upset that maybe it seemed like you were making an arbitrary choice. Or they’re like, “Well, I am going to argue it’s actually this answer”. And so you need a clear piece of information about what the actual resolution is. And that depends on surveillance and the timing of the surveillance. And if you say, “How many cases will be by X date”, but the situation reports comes out three days later, when you fall in the crack between your two outcomes, then what do you do?
If you say, “How many counties will see cases of measles in this month”? Well, did the person with measles drive through that county? Does that count? Was the person diagnosed in one county and then went back home to another county? How are we counting that?
Deaths are not the only health impact of importance
One thing that I’ve been worried about in this response is it seems like when we think about models of COVID deaths and we think about what we’re doing to stay inside to prevent COVID deaths, from a public health perspective, COVID deaths aren’t the only deaths that occur in the US. They’re not the only public health problem that we’re going to have. And so I’m worried about COVID deaths, but I’m also worried about all these cancer surgeries that aren’t happening because we don’t have elective surgeries, you know, that biopsy that didn’t happen. Someone who should have gone to the hospital for a stroke but didn’t feel like they should. All these things. Growing obesity… I do think that these problems that are coming out of the measures that we are taking to prevent the spread of the transmission of COVID… I worry about them. Plenty of people die from being poor. I worry about suicides. We need to think of this from a big-picture perspective and not just do everything we can just to prevent COVID deaths.
Policy change for future pandemics
The fact that “Stay-at-home orders” are actually possible in the US and seem to work… I had not really had a lot of faith in that before and I feel like I’ve been surprised. But I don’t want “Stay-at-home orders” to be the way we deal with pandemics in the future. Like great, it worked, but I don’t want to do this again. And so I think that it has shown us that we need to probably prioritize some other responses, you know, vaccine development, countermeasure development, increasing the capacity of our healthcare system. Because in the US the healthcare system is either profit or nonprofit but, you know, very slim margin kind of operation. You know, it’s hard to have that extra capacity that’s really necessary for something like this. And so that’s really critical.
Emerging Technologies with Potential to Reduce Global Catastrophic Biological Risks
The ones that I think I’m most excited about in the context of this experience with this pandemic is really the easy-to-use ventilators and microfluidic devices because they can sort of solve our problems or at least help solve those problems with rapid and expansive testing. And then also that if hospital capacity is the thing that we’re really worried about not having enough of, then one of those steps is having enough ventilators and having them be something that you don’t have to have specialized training to actually operate.
One type of microfluidic device would be paper-based testing. It’s just a way to do rapid tests that don’t have to go to a lab and that you can get the results pretty quickly. And so I think this could really change the game. Because right now, if it takes a couple of days to get your test and then it takes a couple of days to get your test back, and by the time you get that and you start doing contact tracing, you’re already in big trouble. It’s hard to really make a change in the epi curve that way. But if you can say, “I’m starting to feel sick”, and then you take a test and you know immediately, you can tell everyone you’ve been in contact in the last couple of days that, “Hey, you know, you should watch for symptoms or take your own test”. I think that’s a game changer.
Articles, books, and other media discussed in the show
Tara’s recently published work on misinformation
- Article: Misinformation and the US Ebola communication crisis: analyzing the veracity and content of social media messages related to a fear-inducing infectious disease outbreak
- Blog: The challenge of misinformation during disease outbreaks
Center for Health Security publications
- All of Tara’s publications
- Technologies to Address Global Catastrophic Biological Risks (2018)
- Public Health Principles for a Phased Reopening During COVID-19: Guidance for Governors (2020)
- A National Plan to Enable Comprehensive COVID-19 Case Finding and Contact Tracing in the US by Crystal Watson, Anita Cicero, James Blumenstock, and Michael Fraser. (2020)
- The disease prediction policy dashboard from Johns Hopkins Center for Health Security
- Serology-based tests for COVID-19
- CHS first working definition of Global Catastrophic Biological Risks
- Subscribe to Center for Health Security E-Newsletters
Everything else
- Weaponized Health Communication: Twitter Bots and Russian Trolls Amplify the Vaccine Debate by Broniatowski et al (2018)
- ‘There Are Sensible Voices That Are Emerging,’ How Scientists Are Using Social Media to Counter Coronavirus Misinformation by Jasmine Aguilera
- PM Lee Hsien Loong on the COVID-19 situation in Singapore on 8 February 2020
- Misinformation During a Pandemic by Leonardo Bursztyn, Aakaash Rao, Christopher Roth, David Yanagizawa-Drott (2020)
- National coronavirus response: A road map to reopening by Scott Gottlieb, Caitlin Rivers, Mark B. McClellan, Lauren Silvis, and Crystal Watson (2020)
- Helen Branswell’s articles for STAT
- Biosecurity and Pandemic Preparedness work at Open Philanthropy
- Hypermind prediction market
Transcript
Robert Wiblin: Hi listeners, this is the 80,000 Hours Podcast, where each week we have an unusually in-depth conversation about one of the world’s most pressing problems and how you can use your career to solve it. I’m Rob Wiblin, Director of Research at 80,000 Hours.
The Johns Hopkins Center for Health Security is one of the top global institutions working to prevent health disasters by shaping the development of both technology and government policy.
As you’d expect they’ve been working their ass off on COVID-19, but have also been preparing for this moment for over 20 years.
So I was excited to interview Tara Kirk Sell, who did her thesis on misinformation during disease outbreaks and has worked at the Center for over a decade since completing a very successful career in the US national swimming team.
If you’re as keen on the Center’s work as I am, you’ll be glad to know that as of a few weeks ago you can donate directly to the Center for Health Security through the website for the Effective Altruism Funds, which plenty of you are already signed up to.
They also recently added the option to give to the Biosecurity Program at the Nuclear Threat Initiative in Washington DC.
The Effective Altruism Funds system also supports donations to their four expert-advised funds, and direct donations to 28 other organisations that might be popular donation targets for listeners.
Three projects on the list have been featured on the previous episodes: the Alliance To Feed The Earth In Disasters, also known as ALLFED, the Wild Animal Initiative, and GiveWell.
The site is operated by our fiscal sponsor, the Centre for Effective Altruism, and note two of the expert-advised funds have made grants to 80,000 Hours before.
Alright, at the end of the show I’ll have a few random book recommendations for you, so if you’ve enjoyed my past suggestion for things to read and listen to, stick around for that.
Without further ado, here’s Dr Tara Kirk Sell.
Table of Contents
- 1 The interview begins [00:01:43]
- 2 Misinformation [00:05:07]
- 3 Who has done well during COVID-19? [00:22:19]
- 4 Guidance for governors on reopening [00:34:05]
- 5 Collective Intelligence for Disease Prediction project [00:45:35]
- 6 What else is CHS trying to do to address the pandemic? [00:59:51]
- 7 Deaths are not the only health impact of importance [01:05:33]
- 8 Policy change for future pandemics [01:10:57]
- 9 Emerging technologies with potential to reduce global catastrophic biological risks [01:22:37]
- 10 Careers [01:38:52]
- 11 Good news about COVID-19 [01:44:23]
- 12 Rob’s outro [01:51:02]
The interview begins [00:01:43]
Robert Wiblin: Today I’m speaking with Tara Kirk Sell. Tara completed her PhD in public policy responses to emerging epidemics at the Johns Hopkins Bloomberg School of Public Health. She is now a senior scholar and assistant professor at the Johns Hopkins Center for Health Security where her work focuses on public health policy in response to large scale health events such as disease outbreaks, bioterrorism, or natural disasters. The Center for Health Security might well be familiar to listeners as it received a major grant from Open Philanthropy in part to expand its work on global catastrophic biological risks, which we discussed with the Center’s director Tom Inglesby back in episode 27. Among other things, Tara has studied communication in Ebola and Zika outbreaks and is a co-principal investigator for the Center’s disease prediction project, an online platform to collect forecasts about disease outbreaks and test their accuracy. She contributed to Public Health Principles for a Phased Reopening During COVID-19: Guidance for Governors, which came out just last week. She also happens to have won a silver medal at the Olympics, swimming in the women’s 4×100 metres medley relay. And most impressive of all, back in 2008, she was a contributor for episode 18 season six of the US version of “What Not to Wear”. Thanks so much for coming on the podcast, Tara.
Tara Kirk Sell: Yeah, it’s such a pleasure to be here. Thank you for having me.
Robert Wiblin: We were going to speak last month at EA Global San Francisco, but then suddenly, somehow that got canceled, I guess along with every other conference in the world. I’m glad we can now finally have a chat about the thing that caused our previous interview to get canceled. But first, our usual opening question is what are you doing and why do you think it’s very important work? I guess I might be able to guess what you’re working on at the moment, but it’d be interesting to hear more!
Tara Kirk Sell: Yes, it’s definitely COVID-19 all the time. I guess I should start out and say that the Center for Health Security has really been following COVID-19 since the very beginning of the outbreak. I’ve been working on pandemic preparedness for about a decade. And so it’s really crazy to me to think, “Hey, this issue that we sort of worked on and thought about as the future is now here and something we have to deal with now today and that everyone’s talking about it. Everyone has an opinion. My parents have an opinion they like to tell me all about”. And so it’s strange, but I think working on these pandemic issues has now shown to be incredibly important and affects our everyday lives. And hopefully that work will help us get through this or at least help us get ready for next time.
Robert Wiblin: What are your parents’ policy suggestions?
Tara Kirk Sell: Well, at first it was really funny because they’re older and I kept saying, “Really, you should stop going out. Stop going to the fabric store. Stop going to get groceries twice a day”. And they were very resistant and now they’re completely flip-flopped and they don’t think that anything should reopen for a really long time. I’m glad that they’re taking it seriously now. So that’s good.
Robert Wiblin: Yeah, I think I had a similar experience where my mom’s initial reaction was, “Oh, just let it go through. It’s going to be too much trouble to try to stop it”. But I think she’s changed her mind since then. Is CHS just doing anything that’s non-COVID related now, or has it just kind of eaten up the whole organization at least for the next few months?
Tara Kirk Sell: COVID-19 has really taken over everyone’s lives right now. I think we’ve been trying to keep up our work on a couple other things, but it’s hard even to just read our emails at this point. So I have a couple of projects. My misinformation project that I was doing for Ebola has been published now, and so we were kind of shifting that over to COVID, but at least we were able to finish that out. So a few things that aren’t COVID related, but not that many.
Misinformation [00:05:07]
Robert Wiblin: Alright, well speaking of COVID, let’s start by talking about misinformation which has been, I think, one of your main research interests. If I remember correctly, your PhD was about media and policy interactions during Ebola outbreaks in Africa?
Tara Kirk Sell: Mm-hmm, yep.
Robert Wiblin: What has surprised you about the nature or the extent of misinformation that’s going around about COVID-19. Is it kind of more or less than you’d think, or is it about what you would have predicted?
Tara Kirk Sell: So misinformation is something that we see all the time and we’ve also seen these disinformation campaigns that have really started to move into public health. There was a paper in AJPH about Russian trolls and the vaccine debate. So I’m not surprised that we’ve seen this level of misinformation and disinformation in this outbreak. I’m glad that people are paying more attention to it. I think it is a huge opportunity to sow division in the American public and lead to a lot of lack of trust which to me is really concerning. So I think the themes we saw for the Ebola outbreak, we see those exact same things now. You could almost just take the disease name out and replace it and you see many of those same themes. So that wasn’t surprising. But the extent to which we’re seeing it, I guess, is something that’s new and interesting.
Robert Wiblin: Yeah. So you mentioned kind of active disinformation campaigns. I’m curious, what misinformation about diseases? Where does it typically come from? Actors who are trying to sow discord who’re coming up with clever disinformation to spread? Or is it just people who don’t have a clue about medicine who say stupid things?
Tara Kirk Sell: I think it’s both. I mean misinformation is when you talk about something that’s not supported by the evidence that causes people to have the wrong belief. But it might just be a mistake, right? Or the wrong interpretation. Disinformation is more purposeful and that is definitely happening. I don’t want anyone to be uncertain about that. Those things are definitely happening. And this is an opportunity for foreign actors to really cause problems in the US.
Robert Wiblin: Yeah, how do you measure the scale of disinformation and is it possible to tell, I guess, Russia would be an obvious candidate to be doing that, but are there others as well?
Tara Kirk Sell: I mean, I don’t want to point fingers without evidence, but I think that there are countries that have sophisticated abilities to do this type of thing. And so I think that it’s more than just Russia. Oh, you asked how to measure. Do you want me to talk about that?
Robert Wiblin: Yeah, how do you track it?
Tara Kirk Sell: Yeah, so we tracked misinformation and we didn’t differentiate between disinformation in that case. But we tracked that in tweets about Ebola. And we found that about 10% of tweets had either misinformation or were misinterpretations of true information. And so 10%: is it high, is it low? I don’t know. If 10% of tweets out there are basically false, then maybe that’s a problem. But it’s not like taking over the communication landscape.
Robert Wiblin: Yeah. I kind of wished that only 10% of tweets were false. Probably more than 10% are not that good. My amateur impression is that there’s like, I suppose I don’t live in the US, but at least in the UK it seems like most people are on board with the lockdown. Most people think that COVID-19 is a serious problem. I guess I wonder how many practical challenges has this misinformation or disinformation actually created so far and might we expect it to get worse as people get more sick of being confined to their homes and open to alternative narratives?
Tara Kirk Sell: Yeah, I do think that it’s going to get a lot worse. I think that in the US we’re currently at risk of losing about half the population. The trust of half the population and the belief that these public health interventions are actually worthwhile. I mean, misinformation, the thing that it does is that it makes you lose trust in authorities and you’re not as willing to comply with some of these public health interventions that you don’t really like. And so I think that there’s a moving narrative now that this isn’t worth it. And so I am worried about the rhetoric that’s emerging and I think it’s going to be a really tough couple of weeks coming up.
Robert Wiblin: Yeah. To what extent do you think people are mistrustful of authorities because they have actually just been wrong or slow to respond to this? I suppose it’s like, “Oh, authorities have changed their mind on masks. It seems like for a while they were saying, Oh, there’s not going to be a big problem, but then it turned out to be much worse”. And so maybe people are kind of reacting saying, “Well actually, perhaps the federal government or some of these agencies really aren’t that trustworthy”.
Tara Kirk Sell: Yeah. So I teach a risk communication class and I’ll be honest, the federal government has broken pretty much every rule when it comes to risk communication. So they were slow, sometimes not credible, changing their minds, not consistent. All the things that you kind of hope that public communicators don’t do was done in this outbreak. And so I think that people have lost a lot of trust. But I think the thing that’s really important is that we’re all in this together. So if half the people don’t really believe what’s going on, that’s a big problem. It’s not just, you know, “Oh, then you can do whatever you want over there”. I think that it’s something that we should all care about.
Robert Wiblin: Yeah. I saw some, I think, when you were studying Ebola, I saw some statistic that said 25% of people in the DRC think that Ebola isn’t a real disease. How big a problem is that for trying to control a pandemic over there? Can that show us how big a problem it might be over here if people are not bought into it?
Tara Kirk Sell: Yeah, it’s a huge problem. So if you think, “Okay, we have the perfect countermeasure. Or the right vaccine, the right treatment: we have the exact thing that we know exactly what people need to do and they just need to do it. And if you can’t communicate, and you can’t get people to trust you that what you’re talking about is actually real and what you’re trying to tell them to do is actually useful, you might as well not have anything at all. It’s not worth it. So that’s such a critical component: that trust and that communication.
Robert Wiblin: Well, what about the people who don’t think that Ebola is a real thing? I mean, have they not seen anyone have the disease? It seems like it’s quite a noticeable disease. It seems like it’d be hard to deny that it exists.
Tara Kirk Sell: Right? It might be noticeable, but they might attribute it to other causes. There’s all these conspiracy theories that happen in every outbreak. So I don’t know what specifically was happening there if they didn’t see it. But in the US you’re stuck in your house, or other parts of the world for COVID-19 you’re stuck in your house. You might not see anyone getting it. And so it seems very distant.
Robert Wiblin: Yeah. Okay. You mentioned that some of the US authorities haven’t really been following best practice in terms of communicating about COVID-19. It seems like it’s a very hard challenge to communicate well to the public who’s a very diverse group, especially when you have lots of active groups out there trying to spread disinformation and trying to take advantage of any mistakes that you make. What can organizations do to protect themselves and do a good job in such an environment which seems pretty messed up?
Tara Kirk Sell: Right, it’s always tough. Especially when you say, “Okay, you have to communicate quickly and you have to also be right and sometimes that’s really hard to do together. So the other thing you can do is say, “Here’s what we don’t know. Here’s what we’re doing to find out that information, and here’s how our plans might change if we found that information out”. But I think the critical thing here is to be transparent and not try to spin anything because I think people are smart enough to realize when you’re spinning them. And so I never would recommend trying to cover anything up when it comes to communication.
Robert Wiblin: Yeah. What kind of spinning are you talking about? Are you thinking about trying to explain that things are better than they actually are, or trying to pretend that you know things that you don’t?
Tara Kirk Sell: I think it’s trying to pretend that things are better than they are or being over-reassuring. That just down the road ends up biting you because you know the truth comes out and then it is worse than you said or whatever, and I think that then people lose trust. They don’t want to listen to you anymore.
Robert Wiblin: Yeah. That seemed to be an issue early on. Well back in January, it seemed like the mainstream line among experts was, “Don’t worry about it. Not that many people have it. More people die of all of these other things”. Which seemed really misleading to me because obviously the concern wasn’t that lots of people were dying of the disease in late January, it was that many more people would get it in future and so saying, “Oh, don’t worry, don’t panic”, just seemed like it was completely missing the point. And then of course it was setting them up to have to do this 180 a month or two later when it became much more common. Did you also think that it was a bit odd that people were trying to play it down so much early on?
Tara Kirk Sell: Oh yeah. I was really concerned about trust, early early back in February when people were playing it down. How could anyone imagine that you’ve got it all over China and showing up in Europe, that it wouldn’t come to the US. That it wouldn’t spread all over the world. That’s just common sense. I mean no travel ban is really going to be able to actually prevent that. It was in the US already very early on. And so the idea that you didn’t have to pay attention to it and that it wouldn’t actually spread seems to me crazy.
Robert Wiblin: Yeah. So it seems like it wasn’t only… You might understand politicians who don’t know very much about diseases, who are trying to just put a positive spin on things because that’s the instinct that many politicians have, perhaps. But it seemed like it was people who are more informed like epidemiologists. People who do actually understand diseases or medicine, who people were turning to for advice and they were saying, “Don’t worry about it”. What was going on in their minds? Why did they think this was a good move?
Tara Kirk Sell: I don’t know. I’m not as familiar with everyone who was saying, “Don’t worry about it”. But I was in my little cocoon of people at the Center who thought this was a big deal. So I don’t know what was happening honestly. I do think though that there were people saying we shouldn’t panic and I certainly think that that is the correct message. That we should be thoughtful about how we move forward and that we need to collect this information so we can make the right moves. I don’t think that was a problem but yeah, I guess I wasn’t that familiar with many people who were saying, “Don’t worry about this at all” other than politicians.
Robert Wiblin: I think part of what was going on was perhaps people wanted to promote this idea of “Don’t panic” because they were worried that the public would panic and they felt that the way to do that was really to talk down the risk a lot and then it kind of got a bit out of control, but I’m not sure how big the risk of… It seems like what’s ended up happening is much worse than the public panicking in January. Or maybe I just haven’t seen what happens when the public really panics. I guess people panicked later and it wasn’t that bad.
Tara Kirk Sell: Well, in the academic world, we try not to say that people will panic because people are acting in ways that are rational considering the information that they have most often, at least. I mean a few times you can have instances of people not acting rationally. But for the most part, if there are information voids or there’s the sense that things are getting out of control, then people will act in more intense ways. And so that’s what happened because people were over-reassured and then had this smack them in the face.
Robert Wiblin: Yeah. You mentioned earlier that one way for authorities to protect their credibility is to admit what they don’t know. But I suppose there’s kind of a difficult trade off there. Because I suppose admitting what you don’t know, maybe that makes some people trust you more because they’re like, “Oh, they’re being sincere about what they don’t know” and it makes it easier to then change it. To say something different later on because they can then say, “Well, we previously didn’t know and now we do”, and you’re not doing a backflip. But I suppose saying that you just don’t know lots of things might create this world where people then start looking for alternative authorities because they’re saying, “Well, if the CDC doesn’t know all of these things, that’s not very satisfying to me. I have to find someone else who’s going to give me answers”. Maybe false answers. But yeah, is there a difficult line to tread there? Conceding what you don’t know versus saying nothing?
Tara Kirk Sell: Yeah. I think it is difficult for anyone. But I think what you could say is, “Here’s what we think right now, but there’s a lot of uncertainty about it and here’s what we’re doing to sort of reduce that uncertainty and so the answers may change”. I think a lot of it is just framing and sort of admitting that maybe you’re not an expert or you don’t have that level of understanding. I think that’s fine personally, but that’s just my opinion.
Robert Wiblin: Yeah, are there any countries that have done a good job? Misinformation or communication wise?
Tara Kirk Sell: I was really impressed with the Prime Minister of Singapore’s messages that he put out. They were video messages, and they were incredible when it comes to risk communication. They were explaining everything I’ve said here on what you should do in risk communication, and did a great job of foreshadowing how they might change things coming forward. So I was incredibly impressed by that.
Robert Wiblin: Yeah. Maybe we’ll stick up some links to those videos. Sometimes when I was feeling anxious about the situation, I would go back to YouTube and re-watch some of the videos of him explaining things and be like, “Yes, a source of common sense and like calmness in the eye of the storm”: put it on my mental health rotation. What should we think about misinformation that comes from government? Is that something that we should understand in the same way we do with other misinformation, or is that something that needs to kind of be studied within a different framework?
Tara Kirk Sell: Yeah, misinformation can come from governments. I’m not gonna try to cover that one up. It certainly can happen. I think that it’s possible that people can sort of make mistakes, or that information can change over time. But it can come from companies, people, governments, whatever. It can come from a variety of sources.
Robert Wiblin: Do you have any view on what the internet companies should do? I noticed that YouTube and Facebook and actually so many sites now, they’ve got these banners at the top where they’re trying to direct people towards authorities on coronavirus, which here I guess is the public health people in the UK. I suppose over there they’re linking maybe to the CDC. Is that a good step or do you think that people who kind of reject the mainstream narrative are just going to reject those popups as well?
Tara Kirk Sell: Well I do think that those efforts are really valuable, and the changes to the algorithms that they’ve made can make a big difference. But I agree that if you’re someone who rejects mainstream science or the authorities, then that’s not going to be helpful to you. And so I think this is where research comes in and trying to understand the best ways to access these populations who are distrustful of authority. I think that the answer to the problem of misinformation isn’t necessarily that the tech companies should solve it all for us. I certainly don’t want Facebook to determine for me what’s true or not. And so I think that there’s a lot of stakeholders and I think members of the public also have to take a hard look in the mirror and understand and figure out how we’re figuring out what information sources to trust. And I think that there’s a whole lot of stakeholders who need to think about it.
Robert Wiblin: Yeah. Have you seen this paper about… It’s a little bit dark, but it’s, I guess, different mortality rates from COVID-19 in different districts of the US depending on whether they watch Tucker Carlson, the Fox News host, more than they watch Sean Hannity?
Tara Kirk Sell: I saw the abstract to that. I mean, I think it probably has to do with how quickly you were interested in social distancing. Although it could also have to do with the demographics of how old you are and if you’re able to social distance. I don’t know the demographics of those two shows.
Robert Wiblin: Yeah. Just for listeners, they looked at different counties, I think, in the US seeing whether people who watched the Fox News host, Sean Hannity or Tucker Carlson more. Tucker Carlson spent most of February saying that COVID-19 was going to be a massive problem. Sean Hannity spent most of February saying that it wasn’t going to be a problem at all and they noticed that places where people watch Sean Hannity more, the fatality rates were higher, or more people had died of the disease. I suppose I’ve seen enough empirical social science to wonder how good are the methods there? If you went past the abstract, would it really hold up? If it’s correct, it’s kind of startling. Do you think Sean Hannity… in a sense, people will have died. His viewers will have died potentially because he got this wrong. And I wonder how much people will feel that sense of responsibility in the media to get things correct.
Tara Kirk Sell: I think the media should feel a responsibility to get things correct. But in this case I don’t think that that was right and I think it was pretty bad.
Robert Wiblin: Yeah, how can people figure out who to trust? Especially if they want to just go beyond highly confirmed facts that the CDC is putting out and they want to stay abreast of the cutting-edge science in it. Yeah. What are indications that are hard to fake that something is actually credible?
Tara Kirk Sell: So it’s hard because if you’re looking at preprints, you have to have an understanding of how those methodologies work. And if you’re not in that field, it’s hard. I’m in public health, but I don’t know how to parse exactly what to be worried about in particular in a modeling study. So I think trusted mediators are definitely important there. There can be some leading journalists who seem to have really gotten things right but also, you know, I don’t want to plug our stuff too much, but I don’t have anything to do with the CHS COVID newsletter, but I think it is excellent. I get a lot of information from that and try to follow a couple other news sources. But I’m also just run over with so much information. I think that’s a huge problem that’s happening for everyone right now is that there’s just too much to absorb. I think it’s called data deluge. I just have a hard time even keeping up with my emails. So I try to get what I can as the world’s moving at lightning speed.
Robert Wiblin: Yeah. I had that experience in late January/early February. I felt like I could keep up with what was being learned about COVID-19 and then just in March things snowballed so quickly. I wasn’t even able to keep up with the articles that people were literally emailing me rather than just randomly start reading through them. It’s just like, “I give up. I can’t keep track of this. I’m just going to stop trying to be at the cutting-edge and just learn things a month late and that’s going to be fine”. Maybe that’s a sensible approach because there’s so much going on that really all you can do is specialize in some narrow area and really understand that. And a lot of the rest of it just kind of has to pass you by.
Tara Kirk Sell: Yeah, I do think some things you’re just going to have to say, “I’m going to delete that from my inbox”. But I think one thing that can be really interesting now is that there is more information coming out about what’s happening in localities and what’s happening on the ground. So my colleague Amesh Adalja, he’s a clinician, he also works at CHS and so I really value his perspective because it’s first-person. And I think the more that we’re able to understand sort of what’s happening in localities based on the information that’s coming out of them, I think we’ll have a better picture of what’s happening rather than these large countrywide models or whatever that I think don’t have enough granularity to really tell us that much.
Who has done well during COVID-19? [00:22:19]
Robert Wiblin: Yeah. I’ll just plug Scott Gottlieb who contributed to a paper that came out last week about what governors should do and Helen Branswell who’s a journalist at Stat News — actually Stat News as a whole has been pretty impressive, I think, in covering this. I guess it’s kind of an industry magazine for pharmaceutical companies or for the medical industry, and I guess it really does help when journalists have some expertise within the domain of which they’re writing, which is not always the case. But it means that I think they’ve been able to cover stuff that other places have not been able to make sense of.
Tara Kirk Sell: Yeah, she has been great. And then Scott also has a very sensible voice, so I’m glad that he’s been publishing and pushing things out.
Robert Wiblin: Yeah. Are there any institutions in the US that have overperformed how well they thought that they would go and perhaps should they be given more authority to play a big role in future pandemics?
Tara Kirk Sell: I was really impressed with the King County public health department. They were the first to recognize that. I thought they were really on their game. I thought they were approaching some very sensible solutions. Trying to think through things with the understanding of local conditions. So I was very impressed with them. I think that some states have also done a very good job. I think that when we talk about risk communication, I think the risk communication from Governor Cuomo has been excellent. And I also think that Governor Hogan in Maryland, where I live, he was on his game very quick. And I do think that the states have shown leadership, whereas we had some disappointing efforts by the federal government.
Robert Wiblin: Yeah. Do you think more power to respond to pandemics should be devolved down to the state level or, I suppose, I don’t know, more local levels in other countries as well? Or does that just create other problems?
Tara Kirk Sell: Well, in the United States it varies based on Home Rule vs. Dillon’s Rule. Who has the power? Is it to the locals or is it to the state? I do think the states have done a good job and that the more local you can get, the more responsive you can be. But that spreads out response resources. And in some cases now, we have states actually banding together to put their resources together. In an ideal world, I think the CDC would be empowered to do the great work that we know that they’ve been capable of in the past. Right now they’ve been a little bit silenced and I think that it’s important to have a really strong federal public health agency. So kind of a middle of the road answer there.t.
Robert Wiblin: Yeah. I guess I’ve heard a lot of respect for the CDC in the past, but most people seem to have been disappointed with their response to this one. Did they not have the right people or was it political interference in the CDC that made it hard to do their job?
Tara Kirk Sell: I feel the same and I don’t really know exactly what has happened. I used to work with a lot of people there and I still work with some of them. Over the past few years, many people have retired: some people who I think had a lot of institutional knowledge and a lot of capability to manage a pandemic. So I think that there has been a loss there. I don’t know exactly what happened and I don’t know if we’ll ever know. But certainly, the efforts with regard to testing were pretty disappointing.
Robert Wiblin: Yeah. Speaking of testing, do you have any view on the FDA and their performance? I’ve seen a lot of people who’ve been kind of angry with them for seemingly holding up advances in testing or in other medical equipment that maybe we would like to roll out with a lower level of testing or confirmation of how well it works and safety testing and so on because this is an emergency situation.
Tara Kirk Sell: Yeah, I’ve seen that criticism as well. I think that criticism is reasonable. I don’t get too involved in what’s going on at the FDA. To me it’s sort of a black box going on there.
Robert Wiblin: Yeah. Interesting. There’s been some disappointing things in the US, but if you look at the number of deaths across the country as a whole. The amount of contagion across the country as a whole, it actually doesn’t seem to have done that much worse than many other countries. At least on a per capita basis. It hasn’t done well, but it’s not as if we can say, “Oh, this is all the US federal government’s fault”. It’s like, other countries have often done similarly badly despite not having whatever the unique issues are with the United States. And so it seems to me like around the world, governments have been pretty slow to react to this, potentially being weeks behind where they could have been if they were very proactive. And I wonder what’s the reason that governments tend to lag in their response? Why aren’t they running ahead of it? I suppose one thing is you have this exponential growth where in order to get ahead of where the virus is, you have to suddenly 10X your response one week to the next, because it’s amping up so fast and maybe bureaucracy is not designed to do that or people just don’t want to believe that things are going to be so bad. But it seems like there’s potentially quite deep-seated factors that cause things to happen too slow?
Tara Kirk Sell: I think there’s a number of things happening here. One is that the reluctance to admit that something really bad is coming down the road. I think the other is that taking action has its own cost. If we had started saying “We’re going to close all businesses and do all these things” without our testing actually in place, and we had very few cases, I think it would have been hard to justify that even though we know that there were cases all over, we just weren’t testing very well. So it’s a mix of things and certainly it was a difficult situation, but I think that it would have been better to have testing set up earlier so we knew what was going on earlier. We’re not trying to sort of pop in in the middle of an epidemic curve and try to figure out where we are. I think that would’ve made a big difference, and so I think that was part of the slow reaction. But I think another part was just reluctance to sort of do the things that were hard.
Robert Wiblin: Yeah, I guess there’s this interesting paradox that I suppose closing down the economy, it’s very hard to get broad-based support for that until more people have died. Until things are going worse. But of course by the time that’s happening, now you have to close down the economy for much longer to bring down the case numbers sufficiently. I suppose you can see the example of other countries going really badly, like in a peculiar sense, Italy was very helpful for the rest of the world because seeing the carnage there really prompted other people to say, “Oh my God, we’re going to be that in two or three weeks”.
Tara Kirk Sell: Yeah. So when Italy happened, I said, “Whoa, this is actually in a country that has advanced medical care and can’t handle this”. And we knew that it was going to be bad, but Italy really showed how the case fatality rate changed when you didn’t have appropriate medical care and you had an older population. And so I think Italy was a big wake up call to say this isn’t just less than 1% case fatality. This could be bad if you’re not able to actually handle it with your health system. And that was sort of the wake up call I think for everyone.
Robert Wiblin: Yeah. There’s this funny thing that… I’m originally from Australia and Australia has actually done this quite well. It seems like they imposed lockdown sufficiently earlier. They’ve managed to bring new case numbers down to really low levels already. But then it means that I’m hearing from people that people are losing support for the lockdown, or losing interest in it because not enough people they know have died. So it’s slightly hard to maintain interest in it because they have been so successful at stopping it. I suppose it’s slightly nice that I suppose Sweden, or there’s some countries that are pursuing a slightly heterodox approach where they’re potentially not going to have “Stay-at-home orders” and so we might see some more spread. Perhaps that will be an example to the rest of the world depending on how it goes. Showing like, “Well this is what would have happened”.
Tara Kirk Sell: Yeah. So I think everyone’s tired of being in their house. I’m tired of being in my house. I think it’s going to be very difficult to keep up this communication and ask people to keep doing these things that they just don’t want to do anymore and that they’re not seeing cases in people they know. And so I think that’s going to be difficult. I don’t know if people have to learn the hard way or if there are ways that we can sort of meet in the middle. I hope that that’s the case. It certainly seems like these really thoughtful approaches that public health has sort of put forward as what the gating criteria for moving forward for many states are not going to be met, and people are just gonna do it anyways.
Robert Wiblin: Interesting. I suppose the point of the lockdown was to bring down case numbers. Also to give us time to put in place ways of dealing with a renewed outbreak, like testing capacity or more hospital capacity. Do you think that time has been used well given how expensive it was to buy each day of delay?
Tara Kirk Sell: Absolutely not.
Robert Wiblin: Go on, this sounds good! Well, it sounds terrible…
Tara Kirk Sell: That is a problem with the thing that has been, I guess, most infuriating actually about this outbreak. That we knew it was happening in China in January and nothing was done to really actually make measurable changes on the ground in the US to get ready for it. And then we had it happen in the US, and we all went into lockdown, as you said, at immense cost. Incredible cost to ourselves right now, and to our kids in the future. I mean, this is going to be a big problem for a long time and still, for us, six weeks go by and I don’t see huge improvements in testing capacity in the serology, in PPE, in hospital capacity. These things just haven’t happened and I was sort of wishing that we could have timelines where we say, “This is what we’re going to do by this date and here’s the person responsible and we’re going to take names until we get it done”. I would have liked to see a little bit more urgency in saying each day is many livelihoods. And each day is critical that we push our opening forward one day in a responsible way. And I just don’t think that has happened.
Robert Wiblin: Yeah. What do you think has been stopping it? I suppose I feel sympathetic to the people trying to do this response really quickly because they may just not have very much experience in the area. And I suppose lots of different groups are competing to get protective equipment and maybe the factory is already maxed out and there’s only just so much that the world can do. But it sounds like you think that we’ve underperformed what is realistically possible?
Tara Kirk Sell: You know, I think this is a hard problem and I have sympathy for that. But at the same time, so is how many millions of people we have unemployed. That’s a big problem we have. We have many, many hard problems that we’re dealing with here. And so I just think, you know, we went to the moon, we built a nuclear bomb. That’s a hard problem, you know?
Robert Wiblin: Can’t we make some masks?
Tara Kirk Sell: Yeah, exactly!
Robert Wiblin: Yeah, so are there any specific suggestions of stuff that you think should have been funded maybe that wasn’t funded or maybe regulations that should have been loosened to make things go more smoothly that weren’t loosened?
Tara Kirk Sell: Yeah. So with my public health hat on, I have to say local public health should be funded. The funding for the PHEP program, the Public Health Emergency Preparedness program has really declined in the past decade. Same with the Hospital Preparedness Program. These funding lines are critical and they’ve really lost a lot. So that’s one thing. The other thing is investing in technologies. And I think that we do need to be able to think outside the box and move a number of different technologies forward. I think this is something that the EA community can really help everyone get their arms around what kind of new things that we should be looking at. How do we change the game?
Robert Wiblin: Yeah, it’s interesting. I suppose I’m very optimistic about how things are going to go in Australia because they managed to bring down the case numbers to a pretty low level, and in the meantime, their testing capacity has gone up quite a bit. So now the number of tests they can run per number of cases that they expect, at least over the next few months, is pretty good such that they can do a lot of testing and tracing and probably keep it under control for quite a while. Is it realistic that other countries could have done this as well if they’d had, I suppose, similar capability to expand their ability to respond whenever the “Stay-at-home orders” end?
Tara Kirk Sell: Yeah, so I mean it looks like South Korea has done a really excellent job. They do a great job contact tracing and they’ve had incredible levels of testing. They had a trial run with MERS so obviously they were able to test out what they were doing and improve it and change some laws. And so I think that really did make a big difference. I think New Zealand and Iceland have also done good things. But let’s also now think about the fact that three of these countries are island nations with moderate population sizes. So that makes it a little bit different. These countries have done a good job and I think that the US could emulate that a little bit.
Guidance for governors on reopening [00:34:05]
Robert Wiblin: Yeah. All right, let’s move on and talk about the ‘Public Health Principles for a Phased Reopening During COVID-19: Guidance for Governors’ which CHS put out last week. You were one contributor to that report. What was it trying to say and I guess what was its most valuable contribution in your view?
Tara Kirk Sell: So I think this report was really trying to frame different types of business or activities in a framework that was showing what the risks were as far as level of contact. So was it close contact? How many contacts there were. And then also how modifiable those contacts are. And I don’t think that there was really like specific no-go guidance on that. It was more, “Can we provide people with information that they can then take to a larger stakeholder group and have that discussion about what’s worth it”. There are different levels of risks and sometimes you might take something that might be a little bit higher risk or you have a lot more uncertainty about like schools and you might say it’s worth it, but it’s all in a mix. It’s not just public health who should be making this decision. It should be a mix of stakeholders who bring their expertise into the conversation as well.
Robert Wiblin: Yeah. So I guess I’d been looking for something like this and I hadn’t seen a similar report until this one came out. Maybe there was one out there that I’d missed, but I guess you were kind of trying to rate these different activities, because it seems like we’ve got this whole spectrum, thinking as an economist, there’s activities that create the most disease transmission per util that people derive, which is maybe, I don’t know, a music festival or something where people are in enormously close contact that are probably not super essential that they would do that. And so probably we’re not going to have really crowded music festivals, not going to have a mosh pit for a little while. But then there’s like all the way down to things that we’ve already closed where they’re quite important economically, like people’s livelihoods are being destroyed because they’re not happening.
Robert Wiblin: But the amount of transmission isn’t that great, say, going to a clothes shop that’s not that busy, not that packed. And I guess you’re trying to draw out that spectrum and say, “Well, if you’re gonna open some things, well here’s some things that are more promising”. Either where the number of people you’re close to is not that large, or you don’t spend that long around them. Or you can kind of adapt the shop, say, by saying, “Well, people have got to keep their distance” and then you can reopen the clothing stores. I suppose some of the interesting things are, I guess, shopping malls and retailers seem like they can reopen. I guess parks and actually non-contact sport was one which you’re saying, “Well people could probably play tennis, right”? So we could perhaps be a little bit creative.
Tara Kirk Sell: Yeah. So I mean I pushed for that one because as a swimmer, I was like, “There’s not that much mixing that’s going on when we’re swimming at the pool as long as we’re not breathing all over each other at the end of the lane”. I think it’s pretty clear that ventilation plays a really big role here. We’ve had some studies… I saw a preprint just the other day about the different outbreaks that they sort of tracked in China. And for the most part those have really come from household transmission or from transmission in transportation. And so when people are in very brief contact outside, I don’t see that as sort of a huge risk. And at this point it would be ridiculous to think that we’re trying to strive for zero risk, right?
Tara Kirk Sell: No one lives a zero-risk lifestyle. And so I think that we’re just trying to reduce the level of risk of transmission here. So we want to avoid close contact and we want, you know, not to be indoors. And I think that businesses and people can really think through those requirements and make adjustments. And that’s what I think we should really be striving for here is that people can make these decisions based on the knowledge that they have about the disease rather than these overall orders that sort of compel them to do something.
Robert Wiblin: Yeah. Are you seeing a lot of people responding? I guess I’ve seen a lot of businesses and offices thinking about “How can we reopen”? Because they want to reopen desperately. So they’re thinking, “How can we reopen the office in a way that isn’t going to get our employees killed”? Maybe even in some ways the government response has been a bit disappointing, but perhaps we could see quite a lot of individual responsiveness and flexibility that could allow things to return to some semblance of normality without the disease breaking out again.
Tara Kirk Sell: Right. I do think that businesses have been very flexible and are trying to push for ways that they can do things safely. And I think that’s really great. You mentioned going back to the office. I personally think that probably if you’re able to work from home, that’s one thing that I would say you should probably keep doing if you can do that effectively.
Robert Wiblin: Yeah, I guess maybe in person things construction, perhaps. It’s like warehouses, factories and all that. Also try to figure out how they can keep running. So you said we don’t have much evidence of people catching it from strangers passing by them on the street or in parks or anything like that. It’s mostly in the house, you’re saying, and public transport which are the two key factors. It makes me wonder then–
Tara Kirk Sell: Well that’s from the preprint.
Robert Wiblin: Okay, right. Well let’s just take that as gospel. That makes me wonder… I’ve heard some people who’ve been a bit skeptical about the lockdown because they say, “Well, you’re going to get so much transmission within the household because people are spending tons of time in close contact with their family and housemates then, that given the enormous cost, maybe it’s not actually going to do as much good as you think”. Do you have any view on that?
Tara Kirk Sell: Yeah, so I mean I think people are already in contact with their household and so I mean, I’m not saying I wouldn’t say that that would be a reason to say no on lockdowns, but I do think… I’m not a fan of, like I said, of the lockdown as a coercive sort of measure. I think that providing guidance and helping people understand what should really be done is much better. The costs are immense though. And having people be thoughtful about their contacts I think is important. But even if the lockdown isn’t happening, I’m still having my kids cough in my face. So I don’t know if that’s a huge difference.
Robert Wiblin: I guess part of the reasoning is that as long as you’re with the same people at the same house every day, they can’t infect you twice. So either you get it or you don’t after a while.
Tara Kirk Sell: Right. Although we were social distancing for like two weeks and somehow we caught a tiny cough. Like my whole family and I just…
Robert Wiblin: I’ve been out in the country in this house for like five weeks, seeing practically nobody, and last week I got a cold. I’m like, “Wow, this is incredible. How is this not enough”? You’d think at least if I’m meeting nobody, at least I wouldn’t get colds. But no, it’s not even the case. Yeah, what’s been the response to the report? You mentioned in the notes that librarians weren’t pleased by the suggestion that maybe libraries are a somewhat safe environment to resume normal life.
Tara Kirk Sell: Yeah. So I wasn’t really involved in this debate, although I heard from Caitlin who was the main author of the report that these librarians were saying, “You know, we do have close contact with our customers or with people who are coming into the library”. If you think of it from the perspective of someone who patronizes a library then yeah, maybe you’re not coming in contact. But if you think about a librarian, then they are. I think actually that’s a fair criticism and also something that you could think about for every business. There’s a lot of unique approaches to business and also varying types of contact occurring within those businesses. And so I think an overall judgment can be helpful, but at the end of the day, that’s why we want to have stakeholders involved so that they can articulate those differences and bring them up as important components of a decision-making process.
Robert Wiblin: Yeah. It is an interesting point that I suppose even in a clothing store that’s not crowded, for someone just going there to buy something, it’s probably a pretty safe trip. But then someone who’s behind the counter all day constantly being exposed to different customers, maybe the risk really does add up, and who’s going to want to take those jobs?
Tara Kirk Sell: Right. Well, I agree, but I think also unemployment’s pretty high. People need to make their rent. So then it’s sort of a situation where people don’t have a choice.
Robert Wiblin: Yeah. There was a section in the report talking about the importance of consulting with lots of people in the community before deciding what things to reopen. I suppose there’s an obvious case for that, which is you want to understand people’s preferences about what to reopen and I guess get buy-in from the people who are gonna actually have to do these things that you’re asking them to do. But as I was reading it, I was thinking it could just be that members of the community, like stakeholders in this decision perhaps, don’t have the expertise to really say what activities are risky and which ones aren’t. And they might pressure a politician or pressure officials to reopen something that’s very important to them, not realizing just how dangerous it is. Is there a case for focusing more on people who have expertise in how dangerous are churches, how dangerous is swimming, rather than people who want to go back to swimming?
Tara Kirk Sell: Yeah. So I think that that’s a fair question. I would say though that decision makers need to be able to understand that epidemiology and people who want to advocate for themselves should be able to do so. And then if the decision goes against them, if they’ve at least been part of the conversation and had their considerations thought about. So I think it’s not a problem to have people’s voices as part of the conversation.
Robert Wiblin: Yeah. I suppose as long as the politicians are also paying attention to their public health people. It’s a question of balance and then, yeah, just make sure you don’t listen to only one group.
Tara Kirk Sell: Right.
Robert Wiblin: Yeah. Are there any things that you’re worried will be open too soon?
Tara Kirk Sell: I mean, yeah, there are things. I don’t think that close contact in bars is probably a good idea. It’s an indoor environment. There are a lot of people very close in bigger crowds. Georgia is opening up soon. I think they’re opening up movie theaters. That seems at first kind of dangerous. But I think that there are ways you could modify it, right? If you had people sitting far apart. The same with the gyms. There’s a worry about transfer via fomites, but I also think that there may be ways to modify the situation so that people are safe and that there are a lot of people who’ve been in their houses and we don’t want to increase odds of all these other chronic diseases that can occur from being very stationary.
Robert Wiblin: I guess, yeah, coming into this I would have thought there will have been lots of studies of where people catch colds or where people catch the flu. Like is it at the gym, is it at the pool, is it the church? Is it somewhere else? But it seems like we haven’t really done those studies. I guess when I then think about it, I think, well the way that you might study that is to create some new disease that’s harmless and then give it to people and then see how it spreads throughout the city and where people caught it. But that may not get past ethics approval. So perhaps this is a slightly harder thing to answer than what I thought. But is this kind of research that we just really need to figure out; where do people get the flu the most?
Tara Kirk Sell: It also varies by disease. So then you’re just not sure. And then it’s expensive and hard to contact trace, especially if you have high levels of flu in the community. You know, how many cases of flu do you have and how many times are you exposed? I think it’s pretty tough. There have been studies to see how long a viable virus can be found on certain surfaces. But I’m not sure that those have included infectious dose or that kind of thing or how it works actually in humidity and sunlight. So we’re getting into an area that I don’t know that much about, but I think that those types of things would be really helpful.
Robert Wiblin: So it sounds like a lot of what we know comes from contact tracing early with diseases where we find, in almost all cases, we can track it to someone living with someone or being on public transport or something like that.
Tara Kirk Sell: Yeah. And so there may be a little bit of a bias there because it’s more obvious if you have caught it from your housemate or you know what was going on in public transport. But I think that that’s what I saw in that… I guess I’ll caveat again, in that preprint. And then South Korea has also been keeping track of these things. You know, they had these outbreaks in these churches where there’s close contact. You’re in close contact for a long time. You’re indoors. So I think it’s starting to become more and more clear. There may be risks about spreading the disease in other situations, but that close contact indoors for a long period of time is really the main way that I think people are getting this disease.
Robert Wiblin: Yeah. I guess that’s actually a little bit hopeful in terms of maybe we can reopen a fair few things without letting R get too far above one. If you need close contact–
Tara Kirk Sell: Right, right. I think we have to be careful, but you know it’s possible.
Collective Intelligence for Disease Prediction project [00:45:35]
Robert Wiblin: Yeah. All right. Let’s move on and talk about some other things that are being done at the Center for Health Security. You’ve been a leader on this Collective Intelligence for Disease Prediction project. What is that and how is it similar or different to other forecasting platforms like Metaculus or the Good Judgment Project?
Tara Kirk Sell: Yeah, so it is actually pretty similar. Crystal Watson and I had started and done a past prediction project where we were actually doing a prediction market. But it’s actually really hard to have people who aren’t really that experienced and have a different sort of infectious disease day job to do commodities trading on an infectious disease outcome and so we switched it to a platform that does a lot of the work for them. And this was different from the other platforms in that it was really just specific to infectious disease; there are other questions on those other platforms that are more general. And so we started that up about a year and a half ago with funding from Open Philanthropy and that was a year long project and we were just about to close down in December, but we got additional funding from Founders Pledge and that led us to keep on operating. So one of the goals at the beginning was to establish this platform and we would have the platform set up and we would have forecasters ready to go in case there was a pandemic and here we were. We had it set up.
Robert Wiblin: It’s lucky you got that in December. COVID was already spreading.
Tara Kirk Sell: Yeah, exactly. So we were able to field up about a dozen or so more questions about COVID-19. It was actually really interesting because there was a lot of uncertainty. The forecasters didn’t really have a clear answer on some things like “What’s the case fatality rate going to be”. But then in other cases they were very certain. And it sort of shows how hard it is to write these questions because we would put these ranges of cases and immediately forecasters would go to the highest range and then cases were just exploding and it was hard to tell, you know, “Are cases exploding or is our testing capacity exploding”? And so it did give us some new answers there. That this wasn’t just going to increase at a moderate rate that we would be able to go along with. Over time it was going to be explosive.
Robert Wiblin: Yeah. Interesting. Okay. So just to back up, so you set up this platform where contributors could make forecasts about disease outbreaks and had been running for about a year. How many contributors did you have and did they have a lot of experience in the area?
Tara Kirk Sell: We had various numbers of contributors over time, but we’d over a thousand people who signed up. Each question probably got between 60 and 150 forecasters working on it. And so they had varying degrees of expertise, but a lot of them were in the infectious disease world. We sent out some advertisements through ProMED-mail and so got a lot of attention and interest from around the world. And so that was really something that we wanted. We wanted to have this varying experience. We didn’t want everyone to come from the same viewpoint because we thought that we would have stronger forecasts if we had all these different perspectives. And so that’s how we started out. We had a lot of different questions. We started out with other things like Ebola and cholera in Yemen. But at the end it was really all COVID.
Robert Wiblin: Yeah. And this wasn’t a money one or anything like that. I guess, were people doing it for bragging rights or just to be helpful?
Tara Kirk Sell: Yeah, so no, there were prizes. We’re pretty sensitive to how it looks to have people trading on death, basically. I don’t want anyone to ever have that issue. And so there were prizes for people who were the most accurate. But we weren’t doing commodities trading and we just had a prize for one through five and then we had a random draw based on how many points you had for the next 20. And so people were incentivized to do well, but I was hoping to avoid that unsavory look of having people trade on these bad outcomes.
Robert Wiblin: Yeah. As an economist, my reaction is like, “What? You don’t think life is precious enough to be worth trading in prediction markets”. But I think that that may not be the typical response that people have to people making money forecasting awful stuff. Okay. So how did they perform?
Tara Kirk Sell: Well for the most part they performed really well. But the thing that we learned is that it’s not like magic, right? People need to have information to make good forecasts and if they don’t, or if the surveillance information is bad or really biased, then they don’t make good forecasts. And so I think it’s great to have these newfangled ways of getting opinions and thinking about the future. But if you don’t do that traditional epidemiological surveillance, you have a hard time. And so I think that it just says that we need to do surveillance pretty well.
Robert Wiblin: I guess. Yeah, it has the shit in shit out problem. That just if there’s no actual base information collection that they can rely on, then their forecasts can’t be that good.
Tara Kirk Sell: Exactly.
Robert Wiblin: It’s interesting. I was following the Metaculus predictions which were running fairly early on and I kept noticing that they just always seemed to be trending in one direction. I guess good forecasts should go up and down roughly equally or it should be hard to predict where they’re going, but it seemed to just constantly be moving upwards, which made me wonder if there was something broken about the algorithm. That it was constantly trailing. It was maybe using old forecasts or it could just be that maybe it was just a surprisingly large outcome. So we just kept learning more and more bad things. Did you find anything that there was… what’s the term for this… It should be a martingale, which I guess means that you can’t predict whether it’s going to go up or down. Did you find that in your methods?
Tara Kirk Sell: Yeah, so actually some of those questions we actually cross-posted between us and Metaculus and they were great in setting something up so we could compare at a later date. I mean it’s hard to write these questions because you have to sort of think, “Okay, what could the range of outcomes be”? And the outbreak was moving so quickly and we were finding more bad things happening. And so I think that it comes down to the fact that one limitation of these platforms is being able to write a good question. That the question requires a really good forecast just from the person who writes it. And so it’s very, very difficult to do that. And also, the other thing is that when you actually score it at the end, you need to have a clear outcome, right?
Tara Kirk Sell: Because otherwise your forecasters are really upset that maybe it seemed like you were making an arbitrary choice. Or they’re like, “Well, I am going to argue it’s actually this answer”. And so you need a clear piece of information about what the actual resolution is. And that depends on surveillance and the timing of the surveillance. And if you say, “How many cases will be by X date”, but the situation reports comes out three days later, when you fall in the crack between your two outcomes, then what do you do? So I mean it’s really hard to write the question.
Robert Wiblin: Yeah, that’s interesting. Yeah. That’s something that Philip Tetlock has said when we interviewed him. That he would almost like to spend less time thinking about good forecasting and more time thinking about good question-asking. Did you learn anything specific about how you can do this better, or is it just a perpetual challenge that maybe the thing you really want to know you haven’t got an objective outcome for and you have to keep changing the question because the world keeps changing and so the thing you want to know every week is different?
Tara Kirk Sell: Yeah, I mean that’s true. I think the question writing is the hardest part. The forecasting I think is pretty straightforward. But yeah, writing the question in a way that’s not ambiguous… You know, if you say, “How many counties will see cases of measles in this month”? Well, did the person with measles drive through that county? Does that count? Was the person diagnosed in one county and then went back home to another county? How are we counting that? And so we got better at it as we went along because we avoided some of these pitfalls that we experienced early in the project. But it was still incredibly difficult, even till the end.
Robert Wiblin: Yeah. That’s interesting. I suppose when people I know have made bets against one another on predicting things that will happen, very often they’ve decided that there’s no objective way of deciding who will have won. So they just appoint someone who they both like to just decide who was quite closer to the truth. I guess I haven’t seen that many of those bets resolved. Maybe they’ll just end up bickering about whether the arbiter was fair?
Tara Kirk Sell: Are we talking about a Slap Bet Commissioner?
Robert Wiblin: What’s that?
Tara Kirk Sell: A Slap Bet Commissioner? It was from ‘How I Met your Mother’ and they had a bet that the person who won got to slap the other and so they appointed a third party to determine the rules of how it would occur.
Robert Wiblin: Okay. I guess it is kind of like that. I guess Bryan Caplan is an economist who’s made a lot of public bets with people predicting things and actually I’m the arbiter for one of them, which I think it’s not going to come due for another five years or something. So we may… Well actually he keeps a spreadsheet otherwise there’s no chance I’d remember that. But yeah. One thing I wonder is maybe these prediction platforms need to have someone who everyone respects. Who consistently decides who has won, and builds up a track record of having decided in some reasonably fair way what the correct outcome was and maybe even if they don’t, even if people don’t agree with every decision, they think the person overall is reasonable and so it’s worth participating in it. Is that something you’ve considered doing? Having a person who has their reputation on the line of deciding correctly who was right?
Tara Kirk Sell: Yeah. I don’t know who I’d get to volunteer for that. But I mean that seems like a good solution. They would probably have to be pretty impervious to the complaints that would come along with the job.
Robert Wiblin: “Do you enjoy hundreds of people shouting at you on the internet? Then we’ve got the job for you”.
Tara Kirk Sell: Right, exactly.
Robert Wiblin: Yeah. I guess it’s a little bit like being a judge. Yeah. So what’s the next step with this prediction platform? Are you satisfied that it’s kind of useful and worth keeping around?
Tara Kirk Sell: Well. So for right now we’re going into an analysis phase so we don’t have any more open questions. We’ve shuttled our forecasters off to Metaculus and forecasting on that platform. I think right now we need to determine what actually was working, which questions were sort of the best and provided the best outcomes. And also, we’re looking into the characteristics of the forecasters. One thing I’d like to do, which I haven’t had enough time to actually get going, is to set up an interview project where we can interview people: the people who did the best in the various different projects or various different rounds for the project, and see sort of how they were making their decisions. I know that the Good Judgment Project did this and I think it would be interesting to see if there were any differences when it came to infectious disease forecasting.
Robert Wiblin: Yeah. My feeling is that we could do a lot better on disease forecasting, or at least public opinion formation about where diseases are likely to go than we’ve done, and that that would be really helpful. I suppose you were saying earlier that, and I agree with this, that it seems like in late January or early February we totally could have predicted more or less what’d happen. Not with any certainty, but we could have said what has happened is completely plausible, is a very mainline thing. It wasn’t like this came out of left field because I think the earliest stuff was like, “Well, the case fatality rate seems to be maybe around 1% once you adjust for some cases that we’re not picking up, and it seems pretty contagious. Seems like it’s spreading pretty fast. We haven’t really contained something that seems as contagious as this. Certainly not very often. So I guess it will spread around the world and kill somewhere around 1% of people who get it. In a sense, like nothing surprising has happened, and yet it took a month longer really than we should have to start accepting that and reacting to it. And so it seems like having a prediction platform that very clearly sounds the alarm saying “Yes, this may well happen” could help to get people to do something sooner next time?
Tara Kirk Sell: Yes, I do think so. So for this platform, one of the things we were trying to do is just test how accurate it was. Because we can’t have people making decisions off of bad models or bad forecasts. So that was one thing we were doing. We found that for a number of different types of questions it did very well. I would always say though that these forecasting platforms: new technologies or even traditional disease modeling, should really be a decision support tool, but shouldn’t determine what your decision should be and that there are a lot of other things that go into that. And I don’t like the idea of putting all your, I guess I’ll say, eggs in one basket. I think that you always have to think about the information that’s going into these technologies, models, whatever, and then think about how that is going to really bias the results. So all these things I think you should have a lot of different inputs into your decision-making and I wouldn’t recommend making a decision based off of forecasting platform or just one model or whatever. I think we need to really think about the details and the ins and outs of all those things before we decide.
Robert Wiblin: Yeah. One thing that’s interesting is… Maybe I should ask an economist about this more than a public health person, but the stock market is kind of a big prediction market about how the pandemic is going to go. And the stock market seemed to get things really wrong as well. Like throughout February it was pretty complacent about it, even though there was like billions of dollars on the line there. So it suggests that people getting it wrong was pretty widespread. It wasn’t just a handful of politicians.
Tara Kirk Sell: Yeah, I think the stock market… I don’t think that there was a lot of understanding of what was actually happening with the disease. I don’t know why, because you’re right. There’s a lot of money on the line and it just seems like there wasn’t a lot of thought. I think early on my friend who was going on a Moody’s webinar, they were saying that they were just going to have their forecast be that there would be a million cases. And we were at like half a million at the time and it was like this doesn’t make any sense at all. And so I think there was some sort of like, “We don’t want to be too pessimistic in the approach”, which I think was wrong.
Robert Wiblin: Yeah, I guess maybe I’ve seen this happen a couple of times where the stock market just seems kind of blind to real world events that require expertise to properly understand things that stand outside the financial system. It’s not about predicting the Federal Reserve or something like that. It’s about predicting a disease which is not really what financial analysts know the most about. And in those cases it seems to do fairly poorly, I think, because there’ll be like 1% of people who are trading in financial markets who know enough about this and it really draws their attention and they start thinking about it. But that 1% isn’t really enough to move the market as a whole. And so they end up making a whole bunch of money on that occasion from other people who aren’t really paying attention or who don’t understand what’s going on. But I think my inclination as an economist is kind of to trust the financial markets to be like, “Oh the stock market really is a useful indication”. But I think sometimes on questions that are outside the expertise of stock traders, it really doesn’t tell you nearly as much as you would expect.
Tara Kirk Sell: Yeah, I agree. I mean I’m no financial expert, but I think that that’s exactly right.
What else is CHS trying to do to address the pandemic? [00:59:51]
Robert Wiblin: Yeah. What else is CHS trying to do to address the pandemic? You’ve the prediction market thing. You’re running a whole lot of reports. Are there other things going on that it’s worth people knowing about?
Tara Kirk Sell: Oh man, there are so many things going on. You know, there are reports coming out almost every day on different things. Trying to help policymakers make decisions about the future. Plan a sustainable and thoughtful way back. Probably not to normality, but to something that’s more sustainable. So there’s a ton of work going on. I think we’re also, when we have a moment to breathe, we’ll be trying to do more on that this is a policy window in which we need to sort of think, “Okay, what really should we be doing to get ready for next time”? Because there will be a next time. This is not a one-time event. This is actually, in many ways, this is less than the pandemic that I imagined we were preparing for. And so we have shown that even at this level, we’re not ready. And so it shows us there’s a lot of work to be done. And so I think that that’s the next stage. And everyone else is just kind of reacting to what’s happening right now and how to think about the more immediate future. But soon we will be thinking about the next pandemic or the next bioterrorism event that we need to start getting ready for.
Robert Wiblin: Yeah. Do you worry that it might be important to focus on the next pandemic or preparing for the bigger picture now while people are really excited? Because you can imagine maybe we’ll come up with a solution for this specific virus some point in the next year or two and then people will just not be that interested in spending billions of dollars to actually prepare us for more generic antivirals or more generic vaccine platforms that will be able to deal with the next thing rather than just the disaster that we have going on right now.
Tara Kirk Sell: Right. That’s a fair criticism of the way that the United States has responded to biological events in the past. You know, it’s a cycle of panic and neglect. You panic and you respond and try to prepare yourself for the last pandemic or the last disease. And you don’t actually think about what the next one could be, or the most likely one could be, or the worst-case scenario. And so I do think that there needs to be a change in thinking; will this disease change that thinking? I don’t know. I hope it does. But the past hasn’t been an indicator that we learned from these mistakes.
Robert Wiblin: Yeah. It’s not only the US, I mean I think Australia and the UK both only had influenza pandemic plans, which meant that they made a bunch of mistakes because all of their planning was based around influenza as a virus and not around what would SARS 2.0 be like?
Tara Kirk Sell: Oh right. And the thing is, the flu is probably the most tractable of the diseases because we actually have a vaccine and a large scale manufacturing industry that’s ready to go. If you have a vaccine that’s ready to go, and it’s not the flu vaccine, an ability to manufacture that vaccine at a scale that actually helps protect the world seems fairly impossible right now. And so flu seems to be the thing that we’re most likely to be able to handle.
Robert Wiblin: Yeah. I wonder whether some people… It’s perverse, but I wonder whether now is a moment that some people who are currently focusing on COVID-19 should be putting together spending proposals for stuff that will help with the next pandemic before we solve this and before people will start to lose interest. So maybe this is the time to be saying, “We should be spending billions on generic virus production platforms” and getting just tons of stuff through the budget ASAP.
Tara Kirk Sell: Right, I’ve been thinking about that with Michael Montague, it’s just this response is so overwhelming. I’d like to have those things ready to go when people have a chance to breathe, but we’re not quite sure.
Robert Wiblin: Yeah. It seems like a slightly crazy moment to be thinking about pandemics ten years from now. But yeah, a listener wrote in with a question about how receptive people in the US government have been to a proposal and a CHS report to spend about three and a half billion dollars hiring a hundred thousand contact tracers, which seems like it would be a bargain, potentially. Because then you could actually get the rest of the economy… I mean, it sounds like a lot of money. Maybe they’re going to say, “Oh, this is too expensive”. But of course it could save a trillion dollars. I’m curious to know, have people realized the logic there?
Tara Kirk Sell: Yeah. Well $3.5B seems like budget dust at this point, right? So there has been some uptake and a lot of interest in that proposal. Crystal Watson led that report and I think there has been a lot of interest in it. I think also if we’re not able to move technology forward in a way that gets us a vaccine, gets us a countermeasure, gets whatever things that we need, the serology, the testing at however many million tests we need per week. If we can’t get to that level, I think contact tracing may be one of the most tractable things that can be done. If we’re spending a lot of money or we’re losing a lot of money, it makes sense to spend money on contact tracers. We have plenty of people who are out of work who can do this. And that tracking down who might be exposed and who needs to stay inside for a couple of weeks, I think, may be the key to making it so that we can all sort of get out of our houses.
Robert Wiblin: Yeah. I guess if you think about it, even if 1% of the entire workforce is just doing contact tracing, that’s a lot more efficient than having everyone not being able to work at all. I guess maybe the challenge there is people could be irrational and not want to spend the money. But the challenge might be how do you scale up enough people to train them to do something that might be a little bit tricky and a little bit fiddly and give them all of the equipment, given that we’re trying to do this within months?
Tara Kirk Sell: Yeah, I mean people are going to have to be trained. They’re going to have to be smart. They’re going to have to be thoughtful about the way that they go about this. You can’t just have someone randomly sort of try to do it. And so that is the trick to get people trained up. But I think that’s not as hard as all these other things that we’ve been thinking about. It’s not as hard as having everyone be out of work, so let’s just do it.
Deaths are not the only health impact of importance [01:05:33]
Robert Wiblin: One thing you wrote in the notes is it’s important to consider COVID-19 from a big picture perspective and deaths are not the only health impact of importance. What do you mean by that?
Tara Kirk Sell: Yeah. So one thing that I’ve been worried about in this response is it seems like when we think about models of COVID deaths and we think about what we’re doing to stay inside to prevent COVID deaths, from a public health perspective, COVID deaths aren’t the only deaths that occur in the US. They’re not the only public health problem that we’re going to have. And so I’m worried about COVID deaths, but I’m also worried about all these cancer surgeries that aren’t happening because we don’t have elective surgeries, you know, that biopsy that didn’t happen. Someone who should have gone to the hospital for a stroke but didn’t feel like they should. All these things. Growing obesity… I do think that these problems that are coming out of the measures that we are taking to prevent the spread of the transmission of COVID… I worry about them. Plenty of people die from being poor. I worry about suicides. We need to think of this from a big-picture perspective and not just do everything we can just to prevent COVID deaths.
Robert Wiblin: Yeah, I’ve heard from smart people, I guess some economists, smart amateurs, who kind of think about this intuitively and they’re like, “Well, this number of people will die from COVID-19 but won’t even more people potentially die from the response, as you’re saying from people not doing exercise and people losing their jobs and becoming depressed, or just being poorer in the long term because the economy has been so messed with. Has CHS tried to run any numbers on is it possible that we’re going to worsen people’s health overall if we have to keep running these lockdowns for a very long time?
Tara Kirk Sell: We haven’t run anything like that. I think that this is an idea that’s just percolating through the public health community now and so, you know, COVID was a big threat and certainly many people are dying every day from COVID, so I don’t want to minimize that. But I just want to say, “Hey, we gotta think big-picture here and we also have to think about more than just COVID when it comes to public health in the US or in the world.
Robert Wiblin: Completely, yeah. Initially I was very supportive of the “Stay-at-home orders” and I think that they probably were the right call at the time, but there does come a point where a country, if they look at how their preparations are going for the time after that and just generally their state capacity, and they think, “Realistically we’re not going to have the testing capacity or the tracing capacity soon enough” or, “We’re just not going to be able to do the follow through to control the disease after the lockdown period”, that you might have to accept that you are going to end up with a herd immunity strategy. Because the alternative is to lock down the country for 12 months, 18 months. It’s just so impractical and the damage of doing that just gets too high. Where there’ll be other countries where they do have the capacity to keep the disease under control without a lockdown and they can pursue that other alternative approach. I guess if I was thinking about herd immunity strategy and the immense damage that that will do versus “Stay-at-home orders” on and off for 12 or 18 months, it becomes pretty questionable whether that’s worth it in my mind.
Tara Kirk Sell: I think that this is a debate that’s worth having in the public health and larger community. I don’t feel qualified to make that call on what’s worth it or not, but I do think that there might be a middle ground between lockdown and a full on national chickenpox party. I think that if we can encourage people to understand how to reduce their risks, that may be incredibly helpful and having people reduce their mixing, reduce their contacts to a point that we might be able to have the economy running at some percent of normal and be able to control the disease. I don’t really know how possible that is. I think we’re going to have to do a little bit of experimentation to see. Maybe go back and forth. I think also asking people to stay home is different than a lockdown which is just very coercive. In Maryland we had these requests to stay at home. We were working from home. We weren’t mixing. We were not having big groups. And then there was the lockdown order, or the shelter-in-place order or whatever. And to me, it didn’t really make a measurable difference other than I felt really trapped in my house. And I think that psychological difference is actually really important.
Robert Wiblin: Yeah. You’ve mentioned that a few times. That you think it’s one thing for people to stay at home voluntarily versus being told to or being forced to. Is that because people object to it or it just makes them feel worse? Or is it that the coercive part of it is immoral in forcing people to do things against their will. Or maybe that it saps public confidence in the government over time versus something that they’re choosing to do because they just think it’s good?
Tara Kirk Sell: I think it comes from my faith in people and that I think that people are reasonable. If you give them enough information about risks, they can make thoughtful choices that still correspond to the needs in their lives. And so some people may take more risks because they have to. But I will admit that that’s kind of a rosy picture of other people. And other people may not have that faith. And so that might be wrong. And I think that’s certainly possible that a lockdown order is necessary. Otherwise people make bad choices. But I would like to have more faith in people because otherwise the lockdown orders aren’t going to be something we can do for 18 months. And we’re not going to have a vaccine. And we’re not going to have the testing that we need. So at the end of the day, we are going to have to trust people to do the right thing. So we’ve got to communicate and make it so that that can happen.
Policy change for future pandemics [01:10:57]
Robert Wiblin: Has the response affected your views on what policies are necessary or should be prioritized for next time?
Tara Kirk Sell: The fact that “Stay-at-home orders” are actually possible in the US and seem to work… I had not really had a lot of faith in that before and I feel like I’ve been surprised. But I don’t want “Stay-at-home orders” to be the way we deal with pandemics in the future. Like great, it worked, but I don’t want to do this again. And so I think that it has shown us that we need to probably prioritize some other responses, you know, vaccine development, countermeasure development, increasing the capacity of our healthcare system. You know right now… Because in the US the healthcare system is either profit or nonprofit but, you know, very slim margin kind of operation. You know, it’s hard to have that extra capacity that’s really necessary for something like this.
Tara Kirk Sell: And so that’s really critical. Also PPE… I mean I know that people were storing this stuff up. How did we run out?
Robert Wiblin: It’s crazy. It’s crazy.
Tara Kirk Sell: Yeah, and that we’ve run out of swabs to do the tests in many places. It’s shocking to me. I guess maybe other people wouldn’t be shocked by that when people who really look at it in more depth. But how come we didn’t think that we should have the capacity for that? I think that that’s one thing. That at least one lesson coming out of this is that we should have these stockpiles. And that it’s really valuable to have them and that coming out of this, if you ended up with an extra amount of PPE, maybe you should save it and not try to spend it down.
Robert Wiblin: Yeah, I mean I think the cost of stockpiling PPE is not that high. I mean, if you rotate it through and you just end up having a bunch sitting there in storage warehouses so that doesn’t break down, it seems like it would be a bargain. An idea that I’ve heard is that we need to legalize, and I do actually think this myself, we need to legalize price gouging during emergencies because I don’t know that I trust the government to actually stockpile enough PPE for next time and we need people in the private sector to potentially stockpile this stuff and then sell it at 10 or a hundred times the normal price during disaster so that someone else would do it if our leaders don’t have the foresight to do it themselves.
Tara Kirk Sell: There certainly needs to be incentives. I’m not gonna go there, but I will say that Taiwan has a system where they have a stockpile and then they move things out of the stockpile into use and then put new things back into stockpile. So it doesn’t expire. It’s ready to go. You just have it on hand. And I think that that’s a really reasonable way to go about things.
Robert Wiblin: Yeah, I think fingers crossed we’ll see wearing of surgical masks just by the general public be super normalized which will hopefully then lead to a big increase in our total ability to manufacture PPE so that during a disaster we’ll just naturally produce several times as much as we were before and then we can prioritize healthcare workers during those times. Maybe people have stored up a little bit in their own houses. So there’ll be some natural response, even if the government doesn’t get smarter about it.
Tara Kirk Sell: Yeah, I think at this point cloth masks right now, and then when we have enough for everyone else, it seems like having masks is valuable for source control. I still don’t think that having masks protects you that much, but it could potentially do something in reducing spread from people who are sick. Although I think if you’re sick, you should just stay home. If you’re at super high risk, you should also just stay home. Don’t wear a mask to try to pretend that’s gonna help you.
Robert Wiblin: How do you think the biorisk community is going to be different, if at all, after this? Do you think that people will kind of take it more seriously on a persistent basis?
Tara Kirk Sell: I mean so the bioisk community was taking it seriously.
Robert Wiblin: Oh no, I was thinking will other people take the biorisk community seriously?
Tara Kirk Sell: Oh okay, yeah. I mean, I hope so. It’s strange to have people who don’t do this for like… For the past 10 years, who are really interested in this work. And so I hope that there does continue to be interest and also political interest in moving these issues forward. I do worry that it becomes just commonplace and that people feel all too familiar with it. But I think there are opportunities here for the biorisk community to have a greater say in things. And I think also this has brought up, and this is a little bit of a different question than you’ve asked, but evidence that this type of disease or something similar causes this much disruption certainly should make people aware that there’s a risk for people getting ideas from this and trying to do bad things.
Robert Wiblin: You mentioned face masks. Is there anything that people in the general public should not do if they want to protect themselves or help with the crisis? Are there any mistakes that people are making?
Tara Kirk Sell: Sometimes wearing a face mask can make you touch your eyes or your nose or dig under your face mask more. I mean, I’m not entirely sure what touching your cheek really makes a difference; I’m not absorbing the virus through my cheek. But when the air is coming up out of your mask into your eyes and makes your eyes itch. So we shouldn’t be touching our eyes even though we’re wearing a mask. I mean, I do worry, like I said before, that people will feel like they can do riskier things wearing a mask. If people are like, “Well, I’ll wear a mask when I go see my grandkids and, you know, I’m an older person”. Well that seems like a bad idea. Maybe you shouldn’t go see your grandkids, and wait for a little while until we have a better handle on making sure that you’re safe.
Robert Wiblin: Yeah. On balance I probably am in favor of face masks but yeah, this risk compensation thing does seem like it could eat away a lot of the benefits if people decide “Oh now I’m going to go out a whole bunch more because the mask makes me feel a lot safer to be wearing a mask”.
Tara Kirk Sell: Right. This is a role for risk communication. I don’t want to say that people automatically do this risk compensation, but I think this is a role for communicating with people so they understand actually what they’re doing and why they’re wearing a mask. They’re wearing a mask to protect other people. I think that that’s a critical component there to just have people understand what’s going on.
Robert Wiblin: Yeah. Are there any other lessons that we can learn from COVID-19 that might help us with future pandemics?
Tara Kirk Sell: Hmm. There’s so many. It’s hard to really parse them out. It’s clear that we have a lot of work to do. It’s clear that we need to be able to come to some consensus on some of these measures we’re using to protect ourselves and others. That the debate that was happening in public over masks probably didn’t help. And, I mean, I was part of that debate early on. I really didn’t think that they were that helpful because I was thinking of them as a way to protect yourself. But then when we think about asymptomatic transmission, the fact that someone might be out and about and have the disease and not know it and still be able to spread it, that changed things. Probably my own messages on that could have been improved by saying we might learn more but it might be different. So I should take my own advice there.
Robert Wiblin: Yeah, that seems like it was a little bit of a fiasco. I guess maybe the public health community was a little bit too confident about the… Or they wanted to give a simple message and they thought that that was the right message, but then maybe there wasn’t a lot of flexibility about changing it later on if evidence came in that was different.
Tara Kirk Sell: Yeah. The lessons I’ve already talked about them a little bit but that, you know, testing and understanding what’s going on with the epi curve are really critical. Like taking these guesses and having the information that’s coming in be so biased by your testing protocols. And also having those testing protocols be different everywhere. So you can’t even compare different sets of data to each other. It’s just really problematic. We need to have serology testing much earlier. I think that this is something that really needs some work.
Robert Wiblin: Yeah. One thing I’ve learned is… I suppose maybe I’m a little bit more optimistic about our ability to respond to a very deadly new pathogen. Like if it was killing 10% of people and it seems like we really would potentially just do a full lockdown very early, which’d buy us some time, which I hadn’t really realized that we’d be willing to go quite as far as we have gone in some ways. On the other hand, it seems like any new outbreak, that even one that’s not that deadly, just imposes this enormous economic disruption more than I would have guessed. I would have thought, “Oh, well something that kills half a percent of people who get it probably it’s not going to cost tens of trillions of dollars to deal with that”. But it has, I guess, because we’re choosing to do this big response which might help, but it means that the financial cost is enormous. I guess it seems like it might change the cost-benefit analysis for preparing for this kind of thing going forward because it’s so easy to quantify financially and in terms of tax revenue, the cost of not being prepared.
Tara Kirk Sell: Right. If the cost of not being prepared is trillions of dollars to our economy, maybe we should spend that money on being prepared.
Robert Wiblin: Yeah. Maybe we should put some masks in a cave. Yeah, hopefully that will get through to politicians in the future more. What’s another example? I suppose the UK had some of the best modeling for dealing with pandemics that was out there, but I guess it hadn’t been funded enough or they hadn’t thought ahead enough to make it very flexible and have it be checked and kind of open source so that you could very quickly get lots of people trying to produce different models of the new disease and cross-checking it and things like that, in the sense that the UK deserves credit, because it had sufficiently good disease modeling that other countries were looking to it for advice. But even there, we hadn’t prepared ahead to think, “Wow, we’re going to need these results really quickly within weeks, and it could be something that’s quite unexpected”. I really hope that that kind of stuff gets more funding.
Tara Kirk Sell: So yeah, it’s clear that having good models early on is really critical. And I will say that it’s also really important to have… You know, we talked about this already, to have good information to go into those models. And understanding what biases might be happening because of the different ways that you’re testing. So I think that’s important. Now it’s clear that policymakers are looking to modelers to help them make decisions. And so that’s not going to change. But having good models upfront is really important, as long as we understand that they’re just models and that they’re going to help us make decisions, but I would not say that they’re a perfect prediction of the future and would always caution against that.
Robert Wiblin: Yeah. Something that occurred to me a couple of weeks later maybe than it should have, is that in a situation like this where you’re trying to respond very quickly on the fly to something that’s a bit unpredictable and very uncertain, relying on sophisticated models can potentially lead you astray relative to following heuristics. Like, let’s just do what other people have done, or let’s do what’s worked in the past, or let’s do the thing that preserves option value. I guess this is the thing that I think you find in decision-making literature. That the more complex and uncertain and volatile a situation, the less you want to rely on any kind of very specific sophisticated model to guide your decision-making. Do you think there’s something to that?
Tara Kirk Sell: Yeah. Decision-making: Crystal Watson at our center is the person who really does a lot of that. But I do think there are other ways to make decisions and I think that we should sort of try to get all the information together. One thing that really has happened in this outbreak is that China experienced the outbreak first and so for the most part, everyone has tried to copy China and I was worried that we wouldn’t be able to do it because we don’t have the same testing capacity, the same ability to contact trace and sort of enforce people staying inside. Now certainly we’ve seen a lot of people stay inside, but China was able to move on to the next phase. And so I think when you put these things in place, you need to be able to think ahead to say and then what? And, you know, okay, so we did lockdowns. Now what are we going to do? Well, how do we get out of it? And so I think that that’s a critical piece of making decisions about an outbreak response is that, you know, you’re responding to the threat of the day, but you also think ahead about what are our next steps. And so we need to be able to have those things that help us take those next steps, which we don’t yet.
Emerging technologies with potential to reduce global catastrophic biological risks [01:22:37]
Robert Wiblin: Yeah. All right. Let’s push on from COVID-19 specifically and talk about a report that you contributed to from back in 2018 which was called “15 Emerging Technologies with Potential to Reduce Global Catastrophic Biological Risks”. What are some of the technologies in there that you thought were particularly exciting or yeah, would you like to describe what the main message of that report was first, perhaps?
Tara Kirk Sell: Yeah. So this report was a way of thinking about GCBRs or global catastrophic biological risks in a more positive way. So when you think about these risks, a lot of times the writing and the thinking is very dark. It’s like so many millions of people could die and it’s going to be the end of the world and here’s the disease that’s going to kill you, et cetera. And so here we were trying to say, “Okay, what’s the other side”? What’s the positive side of this? How could we actually meet this threat in ways with technologies that are really going to change the game”. And so we came up with 15 different technologies that came in different phases of an outbreak, from disease detection to diagnostics, and then how we’re manufacturing countermeasures, distributing them, and then, you know, how we’re actually caring for people.
Tara Kirk Sell: And so we had a range of different technologies in these different areas and some are probably closer to reality than others. The ones that I think I’m most excited about in the context of this experience with this pandemic is really the easy-to-use ventilators and microfluidic devices because they can sort of solve our problems or at least help solve those problems with rapid and expansive testing. And then also that if hospital capacity is the thing that we’re really worried about not having enough of, then one of those steps is having enough ventilators and having them be something that you don’t have to have specialized training to actually operate.
Robert Wiblin: Right, yeah. I was going to say I was surprised you said ventilators, because it seems like a lot of people think that the bottleneck is going to be people to operate them, where it seems like you need really experienced nurses and medical professionals to do that. But I guess… So you think it’s possible to produce ventilators that an amateur might be able to operate to a sufficiently good degree?
Tara Kirk Sell: Well that’s the vision. I mean, I don’t think that we’re there yet. You do need to know how to operate the ones that we have right now. So it’s not just producing more ventilators like we have, but producing ventilators that a range of people can operate because the bottleneck is the staff. There are a number of staff members like you said.
Robert Wiblin: Yeah, I’ve heard some people claiming that by the time people get onto ventilators, most people die even if they get ventilation. And so maybe ventilators aren’t as helpful as we think and we should be trying other treatment options. Yeah. Have you looked into that one at all?
Tara Kirk Sell: So people mentioned it actually in our call this morning, that in some hospital systems, it seems like a large number of people on ventilators end up dying. But that isn’t reflective of what’s happening all across the country. And so in other places it seems like they’re able to get people off the ventilators. But having the ICU capacity to take care of these people, and ventilators are part of that story. That’s why we’re doing this social distancing. We’re doing it so that we don’t overwhelm hospital capacity. And so if we’re trying to manage one side of the equation, perhaps we should try to change the other side of the equation.
Robert Wiblin: Yeah, that makes sense. You mentioned microfluidic devices. What are they, and why might they make a really big difference?
Tara Kirk Sell: One type of microfluidic device would be paper-based testing. It’s just a way to do rapid tests that don’t have to go to a lab and that you can get the results pretty quickly. And so I think this could really change the game. Because right now, if it takes a couple of days to get your test and then it takes a couple of days to get your test back, and by the time you get that and you start doing contact tracing, you’re already in big trouble. It’s hard to really make a change in the epi curve that way. But if you can say, “I’m starting to feel sick”, and then you take a test and you know immediately, you can tell everyone you’ve been in contact in the last couple of days that, “Hey, you know, you should watch for symptoms or take your own test”. I think that’s a game changer.
Robert Wiblin: Yeah. Is that one for COVID-19 specifically or is that something that you think could make a really big difference just with all future pandemics if we can make that standard?
Tara Kirk Sell: I think all future pandemics. I think we’ve seen that the diagnostics and the understanding of what’s going on with the disease, reducing that uncertainty is really critical for making good decisions. And so much of that comes from having good and rapid tests.
Robert Wiblin: What’s stopping us from having these tests now: the microfluidic tests that don’t need to go to a lab?
Tara Kirk Sell: This is getting actually outside of my area of expertise, so I’d refer you to the serology report that just came out from the Center.
Robert Wiblin: We’ll stick up a link to that.
Tara Kirk Sell: Yeah. I think that that’s probably a good place for people to go look and see some sort of good testing that’s coming out. I don’t really know exactly what the problem is, but I don’t think that we’re there yet.
Robert Wiblin: Yeah. Are there any technologies from that 15 emerging technologies to reduce a GCBRs report that you’re interested in, or think it would be fun to describe to the audience? One that I was particularly interested in was the idea of vaccines that spread virally. Has that one also drawn interest from others?
Tara Kirk Sell: Yeah. So the cell spreading vaccines are ethically fraught but really interesting, right?
Robert Wiblin: Yeah, right. Exactly. Oh, I could just imagine the reaction from some people on Twitter. How are you going to get that one past the institutional review board?
Tara Kirk Sell: You certainly can’t get consent from someone who’s getting the vaccine this way. So I think that the original idea was that you could vaccinate animal populations this way pretty easily if you had an animal disease. I don’t know how to get over those ethical hurdles as far as doing it in people. It might be a “break glass” kind of thing in case of emergency. But that was just an idea that we thought was really interesting, that you can give a vaccine to one person and that you don’t have to deal so much with the distribution problem. But like I said, huge ethical problems there. And I don’t know how you’d get that through the regulatory process either, but valuable enough of an idea just to at least bring up.
Robert Wiblin: Completely. Yeah, it’s a fascinating one. I suppose the idea is well, what if you could take the COVID-19 virus and then change it so that it doesn’t actually do people any health damage or like very rarely does, and then get that one out there. Then that’s going to spread around and just inoculate people against it. And is it that much worse? In the alternative world, they’re going to get this other disease, probably. So I suppose, yeah, it is ethically fraught, but there’s also a common sense way in which doesn’t this make a whole lot of sense?
Tara Kirk Sell: Yeah. So that’s why it’s there. But you know, obviously with the caveat of all these problems.
Robert Wiblin: Yeah, we’re not going to roll that one out next year. Yeah. Are there any other ones that are exciting and worth explaining?
Tara Kirk Sell: One thing that I was working on for this report was robotics and telehealth. And so I do think if you’re worried about a disease that’s like really taken down your frontline practitioners, if you have the ability to see people through telehealth and use… And we’ve already actually been doing this, but if you have people also in hospitals and some of that treatment can happen through robotics, I think that you can reduce exposure to healthcare personnel that you really need to have on the frontlines. And so now that might be something that could really help in a pandemic. I mean, all of these are something that could really help in a pandemic, but that was something that really struck me. You know, you could even do home based care in that case.
Robert Wiblin: Yeah, and the barriers to that one might not be so serious.
Tara Kirk Sell: Right.
Robert Wiblin: Yeah. Interesting. I guess maybe I’ve moved towards thinking that diagnostics is especially important. That if we had a generic platform that could diagnose people, like the nanopore sequencing stuff. I mean, DNA sequencing has become so much cheaper so quickly that you could imagine that we could end up with DNA sequences that are distributed just all over the place, at least in developed countries, that can very quickly figure out whether someone has the tell-tale DNA or RNA for a particular virus and could massively scale up our ability to diagnose people with new conditions. And then we just won’t find ourselves in this horrible situation that we’ve been in, where it takes months to be able to get to a level where we can diagnose even, you know, 10% of the people who have this illness. And that could potentially make a huge difference to earlier control.
Tara Kirk Sell: Oh yeah. Huge difference. And I think it also tells you a lot more about the severity of the disease. We think this is very severe, but we don’t really have a clear idea on the denominator of our cases and deaths. So if we had better diagnostics and we were able to roll them out to everyone who we wanted to test, we could make decisions with a lot more certainty and a lot more faith that that was the right thing to do.
Robert Wiblin: Yeah. And when you don’t have such a bottleneck on the access to tests, then it’s going to be a lot easier to very early get up these surveillance ones, or these randomly sampled ones, where we just test a random thousand people coming in, and then you can kind of figure out what is actually the infection fatality right here much earlier, and is it worth shutting down the economy to stop this? Whereas we had to do that a little bit blind.
Tara Kirk Sell: Right? I mean, I think it was using a public health precautionary principle that we don’t know how bad it’s going to be. We need to do this to sort of take stock. I wish that the time that we spent while we’ve been doing this, we could come out of the other end knowing what actually is the case, but I think we’re still kind of in the dark, and now making the next set of choices in the dark. So diagnostics would really help us figure that out.
Robert Wiblin: Yeah. Another interesting idea in the report was it seemed like the idea of vaccinating people basically using a band-aid. Because currently there’s this bottleneck on vaccination campaigns, which is that very often you need some level of medical training to inject people with a vaccine, whereas what if you could just mail out every year someone the flu vaccine in a band-aid and everyone gets it in the mail and just sticks it on themselves and then it’s done. And it sounded like this isn’t so far off being possible. And that could really increase our ability to vaccinate people very quickly in an emergency.
Tara Kirk Sell: Right. I think that was one that seemed closer than others. And you’re right: what if you could just send these vaccines to everyone? The distribution problem and getting it actually into people would be solved. And so you’d still have to come up with the vaccine and manufacture it, whatever. But this solves a huge bottleneck when it comes to getting vaccines into people. And so that was one that was pretty exciting as well.
Robert Wiblin: Yeah. One that struck me as a little bit odd was using drones to collect samples from out in the environment. I guess by environment it didn’t mean city streets. I think it meant actually out in rural areas or perhaps I misunderstood what the idea was.
Tara Kirk Sell: Yeah, so actually this is something that’s kind of happening already. You’re using drones to catch mosquitoes and then you test them for different diseases and so you could kind of do something like that, or you could use other ways to collect information on what’s happening out there and sort of pull those in so you don’t have to have someone like drive out, take a sample, do whatever, catch a mosquito. And so that’s kind of part of that idea.
Robert Wiblin: Okay. Yeah. I kind of missed that it was catching mosquitoes. I suppose you can–
Tara Kirk Sell: Well it wouldn’t always be catching mosquitoes. Maybe you would take water samples or whatever if you’re worried about what’s happening in the ocean. That kind of thing.
Robert Wiblin: Yeah, that makes sense. And I guess, yeah, other proposals included ways of constructing molecules, which I suppose is important for making vaccines and other treatments. So in order to be able to scale up treatments more quickly, one thing I wondered is why can’t we just get bacteria to make the antigens that match up the viruses that we want people to develop resistance against or develop an immune response to? Maybe I should talk to a biologist.
Tara Kirk Sell: Yeah, this isn’t really my area. We just collected this information for the report, and that was something that we saw as possible. So maybe you could combine synthetic biology and 3D printing, and you could actually have the bacteria create the precursors that you need for the drugs that then you could print basically. So, you know, this is sort of out there stuff. But yeah, I think synthetic biology is actually something that could really be helpful here as well.
Robert Wiblin: Yeah. Well I suppose it’s kind of increasing the risk in some ways, but then there’s all these opportunities for it to help as well and we’ve just got to make sure that we take those as well. Yeah, I wasn’t surprised when you said, that there’s this concern that with global catastrophic biological risks it’s kind of all doom and gloom. And I’ve found that sometimes it’s really hard, I think, to get people to click through to articles about that on our website because it just sounds so negative. Like who wants to read about just another thing that can go horribly wrong. And with this report, I was like, it was all very bright. It was beautifully illustrated. Very nicely designed. It was fun to read about these technologies in a way that it wouldn’t be fun to read about millions of people dying necessarily.
Tara Kirk Sell: Right.
Robert Wiblin: So I guess this was by design to try to get people to be more positive and more hopeful about this issue?
Tara Kirk Sell: Yeah, and to sort of capture the imaginations of people who want to think creatively about these issues to invest in new things that are interesting solutions that might move us forward. As a public health person, I certainly think capability on the ground is important, but investing in these technologies could be a huge opportunity. So we want to think about opportunities as well as risks.
Robert Wiblin: Yeah, whoever illustrated it really deserves some credit.
Tara Kirk Sell: Yeah, definitely. They were great.
Robert Wiblin: We’ll stick up a link for people to have a read. I keep wanting to steal little images from it. So according to your bio, you started at the Center for Health Security back in 2009, and I guess this GCBR, or the global catastrophic biological risk thing seems to really have come into vogue in the last couple of years. I suppose that the ideas were around beforehand, but it’s become a bigger deal I think in the health security space. How have you found that? Do you think it’s going to be a big focus for you going forward or for CHS?
Tara Kirk Sell: So we do a lot of focus on global catastrophic biological risk. Part of that’s funding related. But I think this outbreak actually has shown us that there are steps before that that we need to sort of be able to do in order to respond to a global catastrophic biological risk. So when I came into the field, I mean there was a lot about bioterrorism that we were working on and things have sort of shifted. We opened the areas of things that we’re working on to be more health security. So it’s not just bio. I was doing some nuclear consequence management for a while. That’s a big problem too. That people really don’t feel like they can really take even the first step on. And so it’s been an interesting few years thinking about all these terrible things, I guess.
Robert Wiblin: Is there any resistance from people who maybe think GCBRs, you know, they’re a serious issue, but they’re not super likely, so we should keep focusing on the things that we were before GCBRs became more fashionable?
Tara Kirk Sell: I think that there is that pushback, but I also think as we try to get a handle on GCBRs, I think that that helps us get a handle on these other outbreaks. And so I think that they’re part of a spectrum of the same thing. And so it’s really important to think about both. And I wouldn’t discount one because of the other.
Robert Wiblin: In that report you point out that very often there’s some commercial applications for these technologies that we could develop, but they tend to maybe lag behind where they could be because they’d be really useful to society, but there aren’t that many commercial applications, so who’s really going to put in the effort to get them onto a big scale. Are there any options for addressing that problem other than just getting more government science grants or grants for health security?
Tara Kirk Sell: Yeah. So I feel like this is actually one area where I think the ingenuity and the can-do attitude of the EA community really could have a lot of value. Thinking about how we move these technologies forward. How we can grow interest in them in a way that gets their everyday use sort of more valued. Because that’s the key. If we can get things into everyday use and they’re easy to use in a pandemic. I guess I don’t have the answers here, but I think that this is an area that I’d love to see some creative thinking. The type that the EA community really does so well.
Robert Wiblin: Yeah, I actually know a few people involved in the effective altruism community who have been looking at more commercial applications for diagnostics, trying to find some commercial path from something that we’re almost being able to use, to can we find a way to make this profitable to scale up so that it is available during a pandemic? Yeah, I hope I’ll maybe be able to get one of them on the show in future to talk about their plans for that. Or perhaps they want to keep that under wraps for their business. Do you know any particularly good resources about GCBRs that people should maybe go and read about that aren’t super widely known?
Tara Kirk Sell: Well there’s that original sort of definition paper for GCBRs that we wrote as a Center, and actually it was really a great process in sort of coming to that definition. We had these big meetings together and talked it through what we thought it really meant. And so I think that that’s valuable. But I mean I think some of the work that’s been published on Open Philanthropy’s web pages is really valuable. I looked at the stuff that you guys published and I think it’s great. So I think that there’s a lot of good stuff out there.
Careers [01:38:52]
Robert Wiblin: Fantastic. Yeah. I guess I haven’t left a lot of time to talk about career advice in GCBRs because we’ve done some episodes on it before. We’ve talked to Tom Inglesby and we’ll probably have some more in future. But is there anything that you’d like to highlight to people who’ve been inspired by COVID-19 to think about a career working on global catastrophic biological risks? Like places to go and work, people to study with, or things that they should keep in mind?
Tara Kirk Sell: Yeah, I think one piece of advice is don’t be afraid to get in on the ground floor. I retired from professional sports and came to the Center as an analyst and I counted paragraphs for references. Sometimes you just have to slog through it. And then once you’ve gained that experience, you move up. And so I think that’s one thing to think about. The other is to use your network to make those connections. It’s a small world. It’s hard to get into sometimes. I was lucky. My boyfriend at the time, now husband, his roommate’s dad knew Tom Inglesby, and so connected me when I retired from swimming. He was like, “What are you going to do with your life”? And I said, “I don’t know, but I think this exercise called Dark Winter is really cool”. And he was like, “Well, I know who you should talk to”. And so the rest is kind of history. But, you know, I came to work at the Center and then very quickly realized that I needed a terminal degree also. And so I was working at the Center part-time while I was getting my PhD as well. So there were a number of steps and ladders to climb to get to move through the biosecurity community.
Robert Wiblin: Yeah. So it’s a little bit chancey your conversion from swimming to working on health security.
Tara Kirk Sell: Yeah. I mean that’s what most of life is? It’s chance, right?
Robert Wiblin: That’s true. Yeah. Are there lots of opportunities for people to move from conventional biosecurity into working on global catastrophic biological risks at this point do you think?
Tara Kirk Sell: Hmm, that’s a tough question. I think global catastrophic biological risks are something that many people are growing in their interest for. I think it really depends on where the funding is. It’s hard to do work that’s not funded, and so we’re always trying to build a grant proposal or a contract proposal and that kind of leads the way.
Robert Wiblin: Yeah. I guess at 80,000 Hours we’ve kind of been assuming that the number of jobs in biosecurity and pandemic control might multiply several-fold in the next five or 10 years just because people will have this memory of COVID-19 or, I guess, it will still be going on for awhile. Do you think that’s right? Or is it possible that we’ll kind of forget about it or governments actually won’t put forward the funding that currently they suggest that they might?
Tara Kirk Sell: So I think that funding is required to grow jobs in this field. There’s a limited number right now, and I think that government is going to be where the jobs are going to expand. We do need more people working on this at the CDC. We need more capacity at the local public health. I think that GCBRs are important and something that can be worked on at the local public health level. But I think that people really need to be able to be flexible and work on everything from the local outbreak to a GCBR and sort of have that flexibility of thinking and an approach to grow the jobs out here, because it’s not that everyone’s going to be working just on GCBRs. That would just flood the field. I think that would be tough. But I think it’s clear that we need a lot more work along that spectrum.
Robert Wiblin: Yeah, it’s interesting. I suppose in the past I thought a lot of the work that’d be focused on global catastrophic biological risks could be quite different than other pandemic control. And maybe there are some really important targeted things like regulation of Gain-of-Function research where you probably wouldn’t do that if you were just interested in pandemics in general. And maybe that is a very important issue for GCBR risk reduction. But do you think that for many people, it could just be that the way to reduce GCBRs is just to reduce transmission of diseases in general, or to be able to respond to pandemics in general because, well, anything that reduces transmission of disease means that it’s easier to get R below one in a disaster scenario and a GCBR scenario?
Tara Kirk Sell: Well, I think that, like you said, there are definitely a number of things that are unique to a GCBR scenario. You know, like working on the Biological Weapons Convention. That’s going to be more large scale pandemics. But I just think that for there to be a lot of jobs and a lot of people working in this field, there needs to be a range of things that they can work on. I mean, I work on a range of different things and it allows me to work on GCBRs, but also have a foot in the practical applications of some of these solutions in scenarios that people are going to have to put into their pandemic plans, whatever, like actually what’s happening in practice. And so I think that flexibility is important. But that’s not to say that there aren’t things that are very specific to GCBRs. I don’t want to be confusing people here. But that’s not the case.
Robert Wiblin: Yeah, I guess that’s true. The Biological Weapons Convention and anything to do with, I guess, like deliberate development of dangerous diseases for weapons purposes or something like that, that’s very GCBR specific and I guess could end up being very important or potentially not depending on whether countries end up pursuing that.
Tara Kirk Sell: Right, yeah.
Robert Wiblin: I suppose GCBRs has this niche within health security that we’re especially excited about, but I suppose it’s possible that there could be people who, in the long-term, might want to work on GCBRs, but they won’t be able to get a job in that niche right away. And so just going into health security in general could be a good stepping stone to potentially one day go and work on GCBRs if they think that’s more effective. Does that sound right even now, when it’s potentially a growth industry?
Tara Kirk Sell: Yeah, I think that there are a lot of opportunities and hopefully there will be a lot of opportunities in the future in health security. And so, you know, jeez, just go get your feet wet. It might not be exactly the perfect thing that you’re interested in spending all your time on GCBRs, but grow your experience and, you know, then there are opportunities along the way that you can shift. But I don’t think that there are many jobs right now that are just solely focused on GCBRs.
Good news about COVID-19 [01:44:23]
Robert Wiblin: Yeah, that makes sense. I wrote an article a few weeks back called “Good news about COVID-19” which was very popular because I guess maybe people were looking for some good news about the situation. Has there been any good news in your views? Like stuff that really indicates that things might not be as bad as they look on the surface?
Tara Kirk Sell: Yeah, so I think some of the serology studies that have started to come out recently might indicate that more people have gotten the disease and maybe it was circulating earlier and not causing quite so much of a terrible disruption. I will admit that the sampling for those I’m not entirely sure about. And some of the statistical methods have been questioned. But it is possible that maybe more people have had it than we thought. I think, from a personal note, my husband had flu negative pneumonia in mid February and my son also had pneumonia a little bit before that. And so if it’s been circulating for longer in the community, that could change a little bit of the dynamics of how we understand this disease.
Robert Wiblin: Yeah. It’s a funny situation when way more people have the illness that we think is the good news. But it does make sense because it means it’s a lot less dangerous than we thought, potentially.
Tara Kirk Sell: Yeah.
Robert Wiblin: Yeah. I’ve been intrigued by those results. I keep seeing these studies popping up on Twitter and there’s such conflicting results in different countries and using different methods and different kinds of sampling approaches. It’s an interesting mystery. It’d be a fun research project to try to unravel. Why is there kind of not a consistent picture being painted of how much this disease has spread?
Tara Kirk Sell: Well I think one of the things is actually that the spread of the disease is hyperlocal here. And actually around the world. And so while you might have a certain level of infections across the country, that there may be differences in what is happening actually at the local level in cities and towns, counties, whatever. That there may be a huge amount of variation actually across the country and across the world, and so that may be why we have such different results. But the other thing that also could be happening is a difference in sampling. And so we know that the disease severity is different across different age groups. And so studies that are showing a huge number of asymptomatic people may actually be… I don’t know about the age distribution there, but I suspect that you have more asymptomatic cases with a younger sample.
Robert Wiblin: Yeah, that makes sense. Yeah. There was a study recently in New York where I think they were sampling all women who were coming in to give birth at hospitals, and they found that… Was it 15% or something from memory, had the condition, which is alarming. Although I suppose New York, we know that it’s been pretty widespread there and I guess possibly pregnant women have been coming into hospital related to the pregnancy and perhaps they’ve been catching it there, or they’ve been forced to leave the house when other people have been in lockdown.
Tara Kirk Sell: Yeah, I mean I guess a pregnant woman is forced to leave the house to go to her prenatal appointments, but at the same time, you’re really trying to cocoon yourself, and the average age of this population is lower than the Diamond Princess group.
Robert Wiblin: Yeah. I guess with the arrival of the serology tests, it’s been really interesting. They’re very hard to interpret as you’re saying, because we don’t know what the false positive rate is there. And so if you get, say, a result saying 2% of the population has this and it’s possible that the false positive rate is around 2%, then you really don’t know how to read that result. And so hopefully we get some more clarity on that in coming weeks and months as we get bigger testing of these kits with known negatives.
Tara Kirk Sell: Yeah. Larger sample sizes and probably a way of sampling the population that pulls in a little more variation or at least can differentiate by age group. I mean, having a large number for asymptomatic cases from the serology or whatever, isn’t that helpful if we don’t know the age distribution, or we don’t incorporate it into our understanding of the age distribution.
Robert Wiblin: Yeah. All right. Well that’s all good news. That maybe there’s some signs that more people have it and so not too many people dying. Well, I would be really happy to find that out.
Tara Kirk Sell: Right, exactly.
Robert Wiblin: I might be a little bit embarrassed because I’ve been skeptical of this theory on social media, so I might have to eat crow if that turns out to be true.
Tara Kirk Sell: I mean, it could be completely wrong, and so I’ll call it my possible good news.
Robert Wiblin: All right. We should probably wrap up. I know you’ve got a busy time trying to do a good job. As a final question, I’m maybe curious to know how has COVID affected your life personally? Are you guys at the CHS getting any sleep, or are you just kind of worked off your feet? I’m not sure whether I mentioned earlier but yeah, you’re responding at 4:00 AM to our planning document for this interview, which made me worry about whether you were getting any rest at all, or whether you just maybe can’t even sleep because you’re just thinking about work all the time?
Tara Kirk Sell: Yeah, well, you know, I think that I might be sleeping more than a lot of other people at the Center, but I was up in the middle of the night trying to work on the notes here for this episode. Sometimes you just wake up and you’re like, “I could lay in bed and waste another hour just laying here or maybe I should just get up and do something”. So that’s what was going on there. The workload has been really intense because it’s COVID-19, but then trying to keep up with normal assistant professor activities. I’m teaching a class. I have students who need help. And my kids are at home with me.
Robert Wiblin: Playing kindergarten as well.
Tara Kirk Sell: Right. I mean I’m glad to have a job. I’m glad to be busy, and I’m glad to have a nice family. I’m in a good situation. But I will say that it has been incredibly intense. Fortunately my husband can help with also being the teacher because my son’s doing online school, but he can’t work a computer by himself because he’s five. So it has been intense, but this family time has also been in many ways really nice beyond the frustrations of trying to get through a mountain of work with your kids just climbing all over you. My daughter who’s three, both of them have become obsessed with David Bowie because they read this little book about him and so they want to listen to David Bowie’s songs all the time and my three year old is singing “Life on Mars” all the time and she loves that line, “Beating up the wrong guy”. And she just loves singing that. So there are moments where it is very funny to be around them a lot. I do want them to go back to school, but there are nice moments too.
Robert Wiblin: Yeah, I guess it’s like there’s the policy analyst side of do you want the schools to reopen, and then there’s maybe the personal side as well where individual considerations could come in. Well yeah. Thanks so much for working so hard to protect us all from COVID-19 and I guess future pandemics as well. Yeah. To you and everyone at the Center for Health Security, I think the work you’re doing is really impressive. My guest today has been Tara Kirk Sell. Thanks for coming on the 80,000 Hours podcast, Tara.
Tara Kirk Sell: Yeah, thanks so much, and thanks for inviting me. This has been really great. I hope everyone has a good listen.
Rob’s outro [01:51:02]
A reminder about the Effective Altruism Funds site which you can use to support the Center for Health Security, among other organisations you might want to help out.
Four random book recommendations you might like. I mostly listen to audiobooks and these are all available on Audible.
The first is The Story of Human Language by John McWhorter, a series of very entertaining lectures about how languages originated and how they really work. McWhorter is one of my favourite writers and always fun in the many interviews he does.
Second is Everybody Lies by Seth Stephens-Davidowitz. The premise is using our Google searches to learn things about us that we won’t readily admit in surveys, like how racist we are or what pornography we enjoy. It’s a good premise to start, but the book really makes the most of it, drawing out some good insights into what people are really like.
Third is Climate Matters: Ethics in a Warming World by John Broome. It considers the moral philosophy of climate change and long-term impacts, including an unusually informed treatment of population ethics. While Broome is an academic I found this one very engaging and easy to follow.
Finally there’s Bolivar: American Liberator by Marie Arana. It’s a cracking book about how Latin America achieved independence from Spain, told through the story of Simon Bolivar, the general who led a series of brutal campaigns across the entire continent to free Venezuela, Colombia, Ecuador, Peru, Bolivia and Panama from colonial rule, over a period of decades.
According to Wikipedia “Bolívar fought 472 battles, of which 79 were important ones, and during his campaigns rode on horseback 123,000 kilometers, which is 10 times more than Hannibal, three times more than Napoleon, and twice as much as Alexander the Great.”
Not too shabby.
Alright, drop me an email if you read and enjoy any of those.
The 80,000 Hours Podcast is produced by Keiran Harris. Audio mastering by Ben Cordell. Transcripts by Zakee Ulhaq.
Thanks for joining, talk to you in a week or two.
Related episodes
About the show
The 80,000 Hours Podcast features unusually in-depth conversations about the world's most pressing problems and how you can use your career to solve them. We invite guests pursuing a wide range of career paths — from academics and activists to entrepreneurs and policymakers — to analyse the case for and against working on different issues and which approaches are best for solving them.
Get in touch with feedback or guest suggestions by emailing [email protected].
What should I listen to first?
We've carefully selected 10 episodes we think it could make sense to listen to first, on a separate podcast feed:
Check out 'Effective Altruism: An Introduction'
Subscribe here, or anywhere you get podcasts:
If you're new, see the podcast homepage for ideas on where to start, or browse our full episode archive.