Allied health professional

Table of Contents
- 1 What’s this based on?
- 2 What is this career path?
- 3 Why do this career?
- 4 Reasons not to work in a health career
- 5 What are the best options among the health careers we considered?
- 6 Who is most likely to succeed in these careers?
- 7 How does it compare to nearby alternatives?
- 8 Should you become an allied health professional?
- 9 How to learn more and test out your potential
- 10 How to enter this path
What’s this based on?
The primary author, Brenton Mayer, who works for 80,000 Hours, drew on his initial training in dentistry and previous experience working as a doctor. We spoke to three people working in these professions and ran a draft of this review past two additional people working in healthcare. We also read existing career profiles on ONET, Prospects and the BLS Occupational Outlook Handbook, as well as some relevant academic literature.
What is this career path?
Rather than being initially trained as generalists like nurses and doctors, allied health professionals are trained to look after a particular set of conditions, and do so mostly independently. For instance, physical therapists can diagnose and treat most causes of joint pain, but if your physical therapist thought your knee pain was caused by something that they couldn’t treat, they would send you to someone who could — perhaps a surgeon.1
Below, you can see a list of the careers we researched. The boundary around “allied health” is vague. We didn’t include clinical psychologists, social workers or alternative health practitioners, even though they’re often included. We did include dentistry, even though it’s often excluded.2 We have separate profiles on medicine and nursing.
Note that the requirements and income vary by country, so follow the links here to get figures for your location:
| Profession and description3 | Study requirements4 | Median income (USA)5 |
|---|---|---|
| Dentists diagnose and treat problems with patients’ teeth, gums, and related parts of the mouth. They provide advice and instruction on taking care of the teeth and gums and on diet choices that affect oral health. | 4 year postgraduate (US) or 5 year undergraduate degree (UK) | $158,000 |
| Pharmacists dispense prescription medications to patients and offer expertise in the safe use of prescriptions. They also may conduct health and wellness screenings, provide immunizations, oversee the medications given to patients, and provide advice on healthy lifestyles. | 4 year postgraduate/6 year undergraduate degree (US) or 4 year undergraduate (UK) | $122,000 |
| Podiatrists provide medical and surgical care for people with foot, ankle, and lower leg problems. They diagnose illnesses, treat injuries, and perform surgery involving the lower extremities. | 4 year postgraduate (US) or 3-4 years undergraduate degree (UK) | $119,000 |
| Optometrists examine the eyes and other parts of the visual system. They also diagnose and treat visual problems and manage diseases, injuries, and other disorders of the eyes. They prescribe eyeglasses or contact lenses as needed. | 4 year postgraduate (US) or 3-4 year undergraduate degree (UK) | $104,000 |
| Physician assistants, known as ‘physician associates’ in the UK, practice medicine on teams with physicians, surgeons, and other healthcare workers. They examine, diagnose, and treat patients. | 2 year postgraduate degree (US and UK)6 | $98,000 |
| Physical therapists, known as ‘physiotherapists’ in the UK, help injured or ill people improve their movement and manage their pain. These therapists are often an important part of the rehabilitation, treatment, and prevention of patients with chronic conditions, illnesses, or injuries. | 3 year postgraduate (US) or 3 year undergraduate degree (UK) | $84,000 |
| Occupational therapists help injured patients develop, recover, and improve the skills needed for daily living and working. | 2-3 year postgraduate (US) or 3 year undergraduate degree (UK) | $80,000 |
| Speech-language pathologists assess, diagnose, treat, and help to prevent communication and swallowing disorders in patients. Speech, language, and swallowing disorders result from a variety of causes, such as a stroke, brain injury, hearing loss, developmental delay, Parkinson’s disease, a cleft palate or autism. | 2-3 year postgraduate (US) or 3-4 year undergraduate degree (UK) | $73,000 |
| Dental hygienists clean teeth, examine patients for signs of oral diseases such as gingivitis, and provide other preventive dental care. They also educate patients on ways to improve and maintain good oral health. | 2-3 year undergraduate degree (US and UK) | $72,000 |
| Diagnostic radiographers7 perform imaging on patients to aid diagnosis. Depending on their specialty they can take x-rays, ultrasound, MRI and CT scans. | 2-4 year undergraduate (US) or 3-4 year undergraduate degree (UK)8 | $58,000-73,000 (depending on specialty) |
| Dietitians and nutritionists9 are experts in the use of food and nutrition to promote health and manage disease. They advise people on what to eat in order to lead a healthy lifestyle or achieve a specific health-related goal. | 3-4 year undergraduate degree (US and US) | $58,000 |
| Respiratory therapists care for patients who have trouble breathing - for example, from a chronic respiratory disease, such as asthma or emphysema. They also provide emergency care to patients suffering from heart attacks, drowning, or shock. | 2-4 year undergraduate degree in the US (doesn’t exist in the UK) | $58,000 |
| Exercise physiologists/sports scientists help patients and athletes avoid or recover from chronic diseases and injuries. They design exercise programs to improve cardiovascular function, body composition, and flexibility. | 3-4 year undergraduate degree (US and UK) | $47,000 |
Why do this career?
The more highly paid professions are solid options for earning to give
The median US earnings for the highest-paid paths are $158,000 for dentists, $122,000 for pharmacists and $119,000 for podiatrists. The top 10% of dentists, podiatrists and optometrists all earn over $187,000 per year, and orthodontists (the specialised dentists who work with braces) earn a mean of $221,000. These are higher incomes than the median for actuaries ($97,000) and software developers ($101,000), and are even comparable to petroleum engineers ($130,000).5
Most of the jobs in the area earn over $70,000, which is still twice the median income,10 and earnings are generally higher than nursing at $67,000.
However, the incomes are still much lower than medicine, which earns a median of over $200,000, but is far more competitive.5
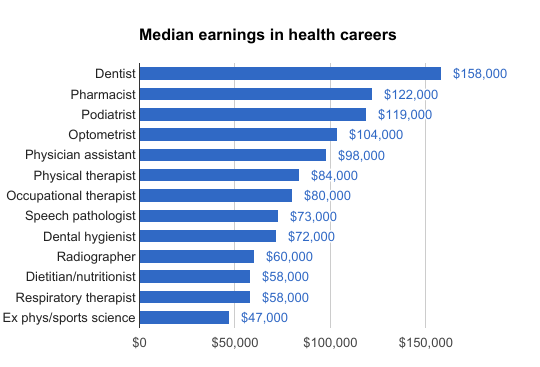
Health professions by median earnings in the USA. (Source: Bureau of Labor Statistics)
The highest-earning paths are the most competitive and take the longest time to qualify for. For example, becoming a dentist in the US requires completing a bachelor’s degree with a GPA of around 3.5, and then a 4 year postgraduate degree.
For those interested in respiratory therapy, the minimum entry requirements are a GPA of 2.5 (or an SAT score in the top 50%), and you can graduate after 2 years.
In contrast, you can be admitted into a respiratory therapist course with a GPA of 2.5 or an SAT score in the top 50%, and graduate after two years.11
In the UK it’s more common for undergraduate degrees to lead directly to work, but earnings are markedly lower — British health professionals earn around half as much as their US colleagues.12 This is significantly lower than the difference in per capita income, which is only about 20%.13
Health is a growth area
Looking at the short term, most health professions are projected to grow 12-30% between 2014 and 2024, far more than the average of 7% for all jobs.
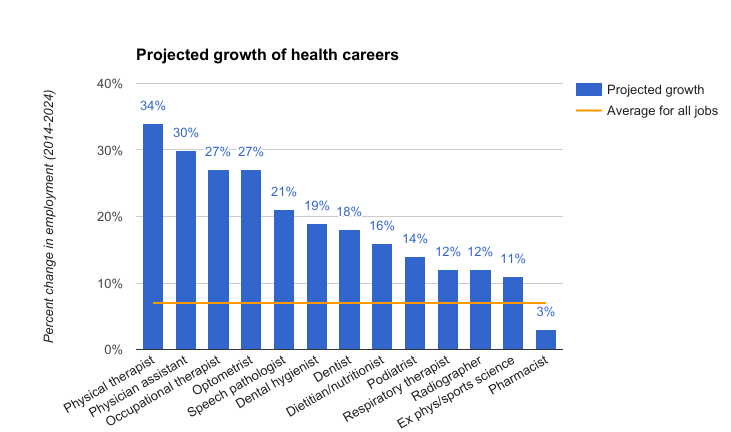
Health professions by projected growth.14 Source: Bureau of Labor Statistics.
Turning to the long term, a study by academics at the University of Oxford suggests that jobs focused on delivering patient care are at low risk of automation in the next couple of decades (you can see the estimates for individual professions here)15. This is because it’s difficult to teach computers to correctly interpret and precisely interact with the changing physical space around them, and it’s even more difficult to program the social intelligence needed to look after patients.
At least two occupations are worth mentioning as possible exceptions to this generally rosy picture:
- Pharmacy jobs are projected to only grow by 3% during this decade, with the Bureau of Labor Statistics predicting a reduction in the number of pharmacists in standard retail settings, as online and mail order pharmacies become more common.16 Speculating further ahead, technology could enable pharmacists to be more efficient, meaning fewer will be needed to look after a given population. More medical and prescription data will be electronically stored (allowing automatic checking for interactions between medications and conditions), and pill packaging and dispensing machines will likely become cheaper and more accurate.17 If this occurs, the effects on employment will probably be felt by pharmacy aids and technicians first, whose jobs are amongst the most vulnerable to automation in healthcare.18
- Studying exercise physiology or sports science leads into a tough job market. Six months after graduating, only 60-70% of graduates are either employed or doing further study in the area.19 Salaries are also the lowest of the health professions we looked into, with many people working in gyms as personal trainers, a position which requires far less education. It’s an unfortunate illustration of some of the pitfalls of ‘following your passion’.
High job satisfaction
Surveys find that most health professions are in the top 25% of jobs in terms of job satisfaction. Physical therapy (a profession which treats a particularly high variety of conditions) fairs especially well, coming in as the second most satisfying job in one survey and the twelfth (out of 274) in another.20
This is what we’d expect since the work does well on all the ingredients of job satisfaction we’ve identified in our research. Allied health professionals directly help people in their work, which is satisfying. The work is also engaging: they have clear tasks with frequent feedback and significant responsibility for diagnosing and treating patients. They’ll work alongside other healthcare workers who they can discuss complex cases with, and they typically have less shift work than nurses and less demanding hours than doctors.
However, there are some negatives. One issue is that several professions, including optometrists and diagnostic radiographers, report a lot of repetition in their jobs, which decreases how engaging their work is.21 Another issue is that many allied health professionals become highly proficient early on and are able to practice unsupervised a year or so after graduating. Whilst mastering your field is good for job satisfaction, doing so right at the beginning and then rarely being exposed to work you find challenging probably decreases job satisfaction. This could be a problem for those professions that have relatively few options for career progression (such as dental hygiene).22
Reasons not to work in a health career
Some positive direct impact, but less than many people think
When working in health, it feels clear that you are helping your patients. Yet, as we explain in the article on medical careers, clinical practice in the developed world only has a modest impact. The key reason for this is that healthcare is already (relatively speaking) well funded in rich countries, so the easy opportunities to help people are already taken, which means additional people and money only have a small impact.
Our analysis was focused on doctors, but we think the impact of allied health professionals is unlikely to be significantly higher.
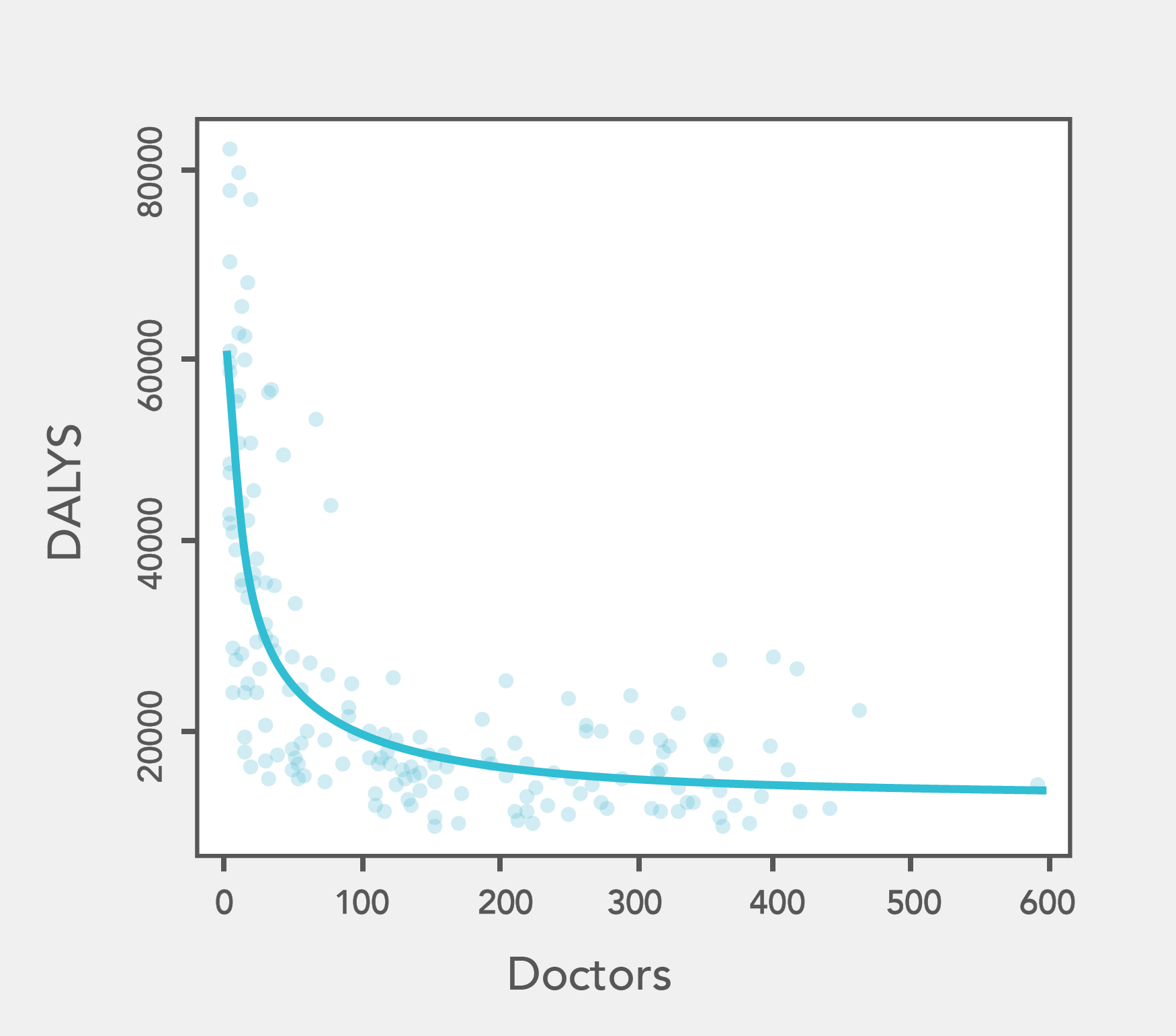
If you wanted to improve health, you could do more good by donating just a small percentage of your income to effective global health charities than by working directly within a rich country.23
If you wanted to maximise your direct impact as a health professional, what could you do?
- Move to the developing world, where healthcare needs are more acute. Our analysis suggests that you could have over 10 times more impact in a developing country because health spending is so much more neglected. Tara, a pharmacist and member of the 80,000 Hours community, saw lots of high impact opportunities to improve healthcare while she was working for the Red Cross. For example, she worked with locals in Bhutan to reduce the rate of drug errors. We would guess that moving to the developing world is most promising for optometrists, dentists and pharmacists. See further discussion in this footnote.24
- Improve the healthcare system. Perhaps you could serve on the board of your profession’s regulatory body, or work in hospital administration. These positions often seem neglected, and can potentially multiply your impact.
- Produce high impact research. With several of these options, you can start researching ways to improve your profession’s clinical practice while at university, and if you’re good at it you could make it a big part of your career. For instance, pharmacists sometimes work on developing new drugs.25 Otherwise, work to excel in your area and develop improved treatments and processes.
Whilst these are possible, note that only a small proportion of health professionals take these routes, and if you’re aiming to get into one of these areas there are likely better ways to get there. Degrees in medicine (for developing world work), health policy (for improving the healthcare system) and biomedical science/medicine (for high impact research) are all probably better options.
Overall, we think that the most promising way to have a big impact through the health careers we’ve reviewed is through earning to give, which is why this profile has been so focused on income and why we generally recommend people take the higher earning options.26
Large upfront investment in training
In the UK, studying a health profession means making a call at a young age that you’ll remain interested in practicing your specialty for long enough to justify the 3-5 years you’ve spent training for it. In the US, you make this decision later in life because the degrees are often postgraduate, but it means a larger financial commitment and more total time at college (often 8 years in total for the most high-earning options).
Narrow career capital
What’s more, this training only prepares you for a narrow role. We normally recommend people build ‘flexible’ career capital early in their career, that is, skills, connections and credentials which will be useful in a wide range of jobs in the future. This is because it’s hard to predict how the job market will change and what you’ll be interested in in the future.
A degree in allied health, in contrast, mainly trains you for a single speciality which exists in a small set of work environments (clinics and hospitals in the developed world). So if you want to leave the career later, you won’t be in a much better position. This could easily happen if your preferences change, you find a better way to have an impact, or if the career does turn out to be vulnerable to automation.
Allied health even compares poorly to other vocational training, such as law, accounting or programming. If you qualify as a lawyer, there are many of types of legal work open to you, and legal knowledge is useful in most sectors of the economy, so even if you decide to leave law, you’ve gained something. Studying maths or economics would be even better again for flexibility.

What are the best options among the health careers we considered?
The following four stand out.
Dentistry
Pros
- Dentistry is the most highly paid of the health professions we considered. In the US, the mean income of orthodontists is $221,000, with a median of $158,000 for general dentists and $171,000 for other dental specialties.27
- Dentistry has the most opportunity for career advancement amongst the health careers we considered. You can become a dental specialist in one of roughly 9 available specialties. This requires several years of study and on the job training. If you don’t specialise, you can earn diplomas or certificates and attend courses on a range of skills which you’ll use in everyday practice.
Cons
- It’s the most competitive – people who are talented enough to become dentists might make a bigger difference in other careers.28
Optometry
Pros
- There may be good opportunities for working in the developing world.24
- It’s also amongst the highest paid. US optometrists earn a median income of $104,000 per year and the top 10% earn over $187,000. UK optometrists earn less than half that, but their training is a 3 year bachelor’s degree rather than a 4 year post-graduate degree.
Cons
- More repetitive than most health professional jobs.10
Pharmacy
Pros
- Well paid in the US, with a median income of $122,000 and the top 10% earning over $154,000.
- Some opportunity for impact by working in research or the developing world.24
Cons
- Poor job market outlook and high chance of automation compared to other health professions.
Podiatry
Pros
- Median income of $119,000 per year, with the top 10% earning more than $187,000. Consultant podiatric surgeons are paid around £80,000 by the British health system.29
- Relatively low competition compared to salary (average GPA of US podiatry students is 3.2).30
- Significant responsibility and variety. Podiatrists can prescribe medication, order diagnostic tests and perform surgery.31
Cons
- There’s less information available on the impact of podiatrists working in the developing world than there is for the above three options.32
Who is most likely to succeed in these careers?
We think most of the social impact of working in these careers will come from earning to give, and once you’re in the job, the pay doesn’t vary that much (in contrast to something like sales, law or finance). So the key question is whether you can get into a university course, and whether you will enjoy the job enough to remain motivated.
The following factors seem to predict success in the health professions:
- High SAT and GPA (Grade Point Average) scores from a previous degree have been robustly shown to predict a higher GPA and completion rate of a health profession course.33
- Several professions have standardised admission tests which are used by universities to decide which applicants they will admit. Some of these have been shown to predict good grades during the health course.34
- Good interpersonal skills, along with an interest in working with and helping people is probably useful, given that you’ll be constantly interacting with the public.
- We’ve noted above that there are relatively few opportunities for career progression in some health careers, which suggests that people with a high need for growth will be less likely to find these options satisfying.
How does it compare to nearby alternatives?
Below we make some very rough comparisons between allied health and nearby options people often consider.
In all cases, the key consideration is your degree of personal fit. If you excel in an area, you’ll gain better career capital, be happier, earn more, have more direct impact, and have a bigger chance of making original contributions to the field. For instance, it’s probably better to be an outstanding nurse than a typical occupational therapist, even though occupational therapists earn more on average.
- If you’re deciding between nursing and these professions, from a social impact perspective, lean towards wherever you can earn the most and donating the extra.
If you’re deciding between medicine and these professions, probably choose medicine. This is because medicine has higher pay and better exit options, plus better potential for doing advocacy, research and work in the developing world.
Software engineering and data science have similar earnings, more flexible career capital and a much shorter training pathway than allied health. If you could enjoy working in one of those areas and be good at it, we’d recommend them over the allied health professions. There are steps to quickly test your potential in software engineering in the full profile.
Sales & marketing/real estate have shorter training pathways and similar average earnings to these health careers. Whilst the highest paid people in these fields do better than the highest in allied health, the spread in earnings is larger, so there’s a chance of earning less. If you’re comfortable with this, have relatively good social skills, and are able to deal with the constant rejection associated with sales, these paths might be better.
Corporate management usually involves more stress and longer hours than allied health. On the other hand the work is more varied, with greater opportunity for career advancement and more flexible career capital. Median salaries are comparable to the higher end of the allied health professions and if you do well it’s possible to earn much more.
Most lawyers (as opposed to those from top firms as considered here) have a similar salary to the more highly paid allied health professions and law is also a good option for those who are strong on verbal skills. It gives you more flexible career capital and a chance to earn a lot more, but the hours are probably longer (particularly at the start of your career) and job satisfaction is lower. We’d recommend whichever you would enjoy and have the best personal fit for.
Again, in all cases, the general pros and cons need to be weighed against how much you’d enjoy the job and how good you’d be at it.
Should you become an allied health professional?
Here are some key questions to ask yourself.
- Could you find working as a health professional satisfying? Would you enjoy near constant social interaction and working with the general public? Does the health profession you’re considering work in a narrow field which you would find repetitive after a decade or more?
Are you comfortable with the idea of earning to give being the main way that you have an impact with your career? Are you reasonably confident that you will follow through with donating a substantial proportion of your future earnings?
Relative to your other options, is this a good option for earning to give? Could you get into one of the higher earning pathways, like podiatry, dentistry or optometry? Could you work in a country which pays health workers well, such as Australia or the US? How does it compare to other options you’d consider?
Do you highly value having a stable job, which isn’t too demanding of your time, either for personal reasons, or so you can do high-impact volunteering? The allied health professions have standardised career paths, strong projected job growth, and usually 40 hour work weeks. If you value these more than the average person, this is a point in favour of allied health.
Most importantly, have you explored other options, so that you’re 80%+ confident that this is the path for you? Becoming a health professional means making a large up-front investment in a career with narrowly applicable career capital and relatively few opportunities for advancement. This makes it really important to explore your other options before committing. Read about how to explore.
As always, if you couldn’t imagine yourself doing anything but working as an allied health professional, you should probably become one.
How to learn more and test out your potential
Before committing to a university course, you can test out your fit for a career in health by:
- Learning more about what the different options involve by reading the BLS and Prospects guides on the professions you’re interested in. You can also look at our wiki which will suggest some more resources.
- Finding out which professions you could get the grades required to enter, because some of the university courses are very competitive.
- Looking into what the professions are like day-to-day by speaking to friends of friends who work in the area.
- Organising to ‘shadow’ someone working in one of these professions for a few days. An ideal setting is a hospital so that you can see what other health care workers are doing and perhaps arrange to do the same with them if you’re interested in their work.
How to enter this path
- Prepare your university application. During your prior education you should be aiming to study all the necessary prerequisite subjects and achieving the required grades. You should demonstrate an interest in the subject through shadowing people or working in a related area.
- Find and follow some advice tailored to the specific course you’re applying for.
- Often you’ll need to take a specific admission test and it’s worthwhile studying specifically for that.
- Finally, apply to a university to train you in your chosen profession.
Notes and references
- Thinking of allied health professionals as ‘non-generalist health workers who independently manage a particular set of conditions’ is a sensible way to start, but it does miss some nuance. Most significantly, 1) in most regions you should think of dental hygienists as working under the supervision of dentists rather than independently. 2) Diagnostic radiographers are experts in taking high quality images for diagnosis, not in diagnosing and treating a set of conditions. 3) Whilst pharmacists do make diagnoses and recommend treatments, you should think of their primary function as ensuring the safe and appropriate use of medications for all conditions, not a subset of conditions. 4) While these health professionals can treat patients reasonably independently, this doesn’t mean that they don’t communicate and work with the rest of the healthcare system. Still, this framework is a useful way to think about how their function differs from doctors and nurses, and we’re sure if you’re seriously considering working in one of these areas you’ll read up on exactly what the job will involve.↩
- Multiple contradictory definitions of ‘allied health professions’ exist, so it’s hard to be strictly correct about the way you use the term (especially here, as this discussion isn’t limited to a certain region which uses a shared definition). We can make some useful generalisations about this group of careers as they are similar along a number of important dimensions (although we’ve included multiple clarifications and footnotes throughout the piece to make it clear which professions our claims apply to). We’ve excluded social workers and psychologists (often classified as allied health professionals) because the nature of their work and the audience interested in doing it seems different enough from these jobs that it could warrant a separate profile in the future. We’ve also excluded alternative health practitioners (also often classified as allied health professionals) because of serious doubts about the efficacy of their treatments and their ability to improve their practice by responding to evidence in the future. Note that many nursing specialties have a reasonably high degree of autonomy and pay, making them similar to many careers listed here. However they do not belong to any definition of allied health, so we’ve discussed them separately in the nursing career profile. Overall, this review considers most healthcare workers educated with an associate’s degree or higher, who are practicing direct patient care and are not nurses, doctors, clinical psychologists, social workers, or alternative health practitioners. We would expect that other jobs which fit these characteristics but which we didn’t research, like genetic counselling or audiology, will have similar characteristics to the ones in this table that we did investigate.↩
- The majority of the profession descriptions are taken directly from the Bureau of Labor Statistics Occupational Outlook Handbook. We have rounded the incomes to the nearest $1000.↩
- If you have an undergraduate degree already (particularly in a related field) there is often a postgraduate degree which you can complete in a smaller amount of time to attain the same qualification as the undergraduate degrees we’ve listed here. We’ve tried to indicate the typical duration of courses rather list a range which all courses will fall into, so our numbers should give you a general idea of the length of these courses, but there will be individual courses on offer that contradict our numbers here. Often these courses have ‘internships’ or similar, in which after you graduate, you are paid but practice under supervision.↩
- Bureau of Labor Statistics, Occupational Employment and Wages (May 2015).↩
- Successful applicants usually have some experience working in healthcare with a related undergraduate degree.↩
- In this category we’re including ‘diagnostic radiographers’ (UK term), as well as ‘nuclear medicine technologists’, ‘radiologic and MRI technologists’ (US terms) and ‘sonographers’. We are not including ‘radiation therapist’ (US term) or ‘therapeutic radiographer’ (UK term).↩
- Practising sonography (the ultrasound specialty) in the UK and Australia normally requires postgraduate study after completing an undergraduate degree in radiography, which means the length of study for this specialty is more like 5 years.↩
- The definition of ‘dietitian’ vs. ‘nutritionist’ is variable. Generally the term ‘dietitian’ connotes more training. The Bureau of Labor Statistics considers them one profession for their income statistics so we have done the same.↩
- Wikipedia article on personal income in the United States.↩
- Source 1 and source 2.↩
- Data from Payscale (which has statistics for both countries), the Bureau of Labor Statistics (USA statistics) and Prospects (UK statistics) all indicate that UK health professionals earn approximately half as much as their US colleagues. None of the UK incomes we looked at were exceptions. The same is true for doctors. Australia’s health courses are as long as the British ones, but the incomes of health professionals tend to be closer to (although not quite as high as) the USA.↩
- Wikipedia pages for US income and UK income.↩
- We arrived at 12% for ‘Radiographer’ by calculating the combined rate of growth of the several professions which make up our classification of ‘Diagnostic radiographer’ (see footnote #6) using Bureau of Labor Statistics data. This has obscured the poor growth rate of the small profession of nuclear medicine technology, which is projected to be 2% between 2014 and 2024.↩
- Frey, Carl Benedikt, and Michael A. Osborne. “The future of employment: how susceptible are jobs to computerisation?.” Technological Forecasting and Social Change 114 (2017): 254-280. See the paper here.↩
- Source.↩
- For example see this article considering the role of tech in pharmacy.↩
- On a scale of 0 (least automatable) to 1 (most automatable), pharmacy technicians were rated as 0.92 and pharmacy aids as 0.72 by the Oxford study we referenced earlier.↩
- Source. People study these degrees to work in health and also to work with athletes. The 60-70% figure comes from a combination of these two areas. Our figures on income and are for ‘exercise physiology’ (which is generally about working with patients), rather than ‘athletic trainers’ (who have a slightly lower median income of $45,000/annum according to the BLS). We have not invested the time in making our advice more precise by determining which courses lean more towards sports and which lean more towards patient care, and we haven’t found a figure on the employment rate of people who study degrees leaning more towards patient care. We think doing so is unlikely to change our general conclusion that doing studying exercise physiology or sports science is rarely a good choice for people who want to have a large positive social impact. This is based on our reading of the area as well as a discussion with someone who used to study exercise physiology.↩
- Source 1 and Source 2 show most health professions in the top 25% of jobs in terms of satisfaction. Source 2 and Source 3 show physical therapy in the second and twelfth places in terms of satisfaction.↩
- ONET surveys have data on this. “Repeating the same physical activities or mental activities over and over, without stopping”, is reported as either important, very important or extremely important by 87% of radiographers and 82% of optometrists. 51% of radiographers said their job required “making repetitive motions” more than half the time. 17% of optometrists said their jobs required “making repetitive motions” ‘continually or almost continually, 30% said it was required more than half the time and 22% said it was about half the time. Source for optometrists and source for radiographers. This issue probably looks less significant for those working in the few US states where optometrists can prescribe and perform minor surgical procedures.↩
- There’s a tradeoff here between the satisfaction of mastering an area and the satisfaction of overcoming challenges. Different people give different weights to the two sources of satisfaction. If your ‘need for growth’ is high this suggests you should look for a job one with more challenges to overcome. See our page on the subject for more on this issue. Source 1 and source 2 for the claim of there being relatively little career progression available in dental hygienics.↩
- Effective global health charities such those evaluated by GiveWell can probably produce a year of healthy life for around $200. Occupational therapy has mid-range earnings for a health career, at $80 000/annum. Giving 1% of that annual income to a top charity should improve health by a similar amount to what an additional doctor in the developed world could do over the course of a year (1% of $80,000=$800. $800/$200=4). See our profile on medical careers for more information on the direct impact of doctors.↩
- We would guess that optometrists are valuable because preventable visual impairment is an enormous cause of ill health in the developing world. There are often highly cost effective solutions to this, such as correcting focusing errors and other interventions available to optometrists. The WHO estimates that US $202 billion is lost in productivity per year just from focusing errors. This paper estimates that the cost of fixing these is on the order of a few hundred dollars per year of healthy life gained. There are several NGO’s which can be easily found online that are asking for volunteer optometrists to work in the developing world.
Fricke, T. R., et al. “Global cost of correcting vision impairment from uncorrected refractive error.” Bulletin of the World Health Organization 90.10 (2012): 728-738. Source.
Baltussen, Rob, Jeroen Naus, and Hans Limburg. “Cost-effectiveness of screening and correcting refractive errors in school children in Africa, Asia, America and Europe.” Health Policy 89.2 (2009): 201-215.
Source.
Dentists can perform low cost, life improving surgical interventions with limited need for follow up (eg. extractions and fillings – more complicated dentistry is less common in these contexts). It’s not clear how cost effective dentistry is in this context. Like for optometry, there are several NGOs which can be easily found online asking for volunteer dentists to go to the developing world.Benzian, Habib, and Richard Niederman. “Cost effectiveness of dental surgery procedures: a call for strengthening the evidence.” World journal of surgery 38.9 (2014): 2484-2485.
Source.
Pharmacists seem to be particularly valued by organisations delivering emergency care such as Medecines Sans Frontieres. Radiography and podiatry are also probably very useful in some developing world contexts too.For each of these, it’s possible you could increase your impact by getting involved in training locals or improving health systems rather than working directly. Doing this well means spending a large amount of time in your chosen location. You need local buy in, to make sure you understand the context well enough that your changes are improvements, to make sure they’re sustained etc. Tara’s experience, was a good illustration of this, as was the author’s experience working as a final year medical student at a hospital in Fiji.
Of the remaining health professions we considered, they generally don’t have treatments that 1) have large effect sizes, and that 2) they can administer to many patients over a small amount of time. Given this, we would expect that their impact won’t be dramatically increased by moving to the developing world, although we haven’t investigated this in detail.↩ - See for example, this article on pharmacists working in academia. There are number of places online to read more about the research done various professions. E.g. The International Association for Dental Research.↩
- This is also because they tend to have more autonomy, which should increase job satisfaction. Note that we don’t think most people should be earning to give as the main way they improve the world.↩
- Source.
Optimising your income for earning to give probably means some combination of:
1) Specialisation – either with a formal specialisation and masters degree as required for orthodontics or prosthodontics (around 10% of dentists specialise like this), or with certificates allowing you to do more lucrative procedures.
2) Creating a stable patient base – staying in one area, perhaps owning your own practice as 25% of US dentists do, and building/maintaining your patient base through excellent bedside manner.
3) Increasing the amount of time you spend doing well paid work – optimising for more expensive procedures (perhaps through learning skills through certificates), working with a dental therapist and a dental hygienist who do less well compensated but still valuable procedures etc.↩ - Source. This table of the secondary scores required to enter dentistry in the UK showed a UCAS range of 406-555. If we remove one a single outlier from the top and the bottom it becomes 460-515. You can use the drop down menu to compare it to other courses to get an idea of how high this is. Similar scores will be required in the US and Australia.↩
- Source.↩
- Source.↩
- On an ONET survey 80% of podiatrists reported they had ‘a lot of freedom’ to make decisions, the highest of any of the health professions we looked into. The surgeries they perform are quite significant, including joint fusions and inserting pins into bones.↩
- We’re not too sure how impactful podiatry would be in the developing world. There are fewer groups online looking for people to volunteer overseas as there are for the preceding 3 professions we mention, and MSF doesn’t list podiatry as a priority for employment (but it’s also a smaller profession than the others). Podiatrists treat a lot of chronic conditions and disorders of movement, which might be hard to make a big impact on. On the other hand, they also perform surgeries, which can do a lot of lasting good. It might be possible to find ways to just do high impact podiatric interventions, but we haven’t investigated this fully.↩
- Though also note that high academic achievement predicts success in many careers and so shouldn’t really push you towards the allied health professions over other careers. Source 1, source 2, source 3, source 4.↩
- This paper found it was useful for optometry. This paper found it was useful for medicine.↩